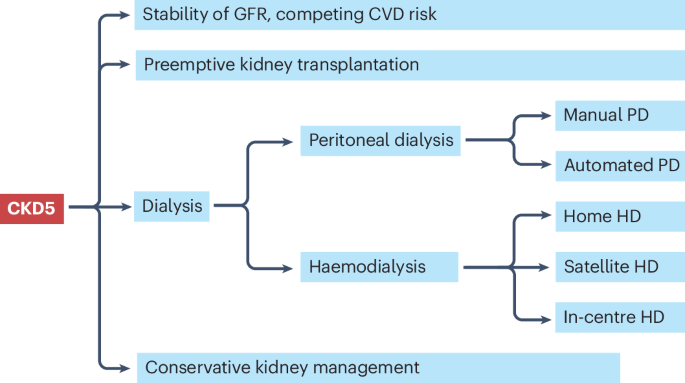
Optimal patient care in advanced chronic kidney disease progressing to kidney failure
Kidney Disease: Improving Global Outcomes (KDIGO) CKD Work Group. KDIGO 2024 clinical practice guideline for the evaluation and management of chronic kidney disease. Kidney Int. 105, S117–S314 (2024).
Google Scholar
Levin, A. et al. Executive summary of the KDIGO 2024 Clinical Practice Guideline for the Evaluation and Management of Chronic Kidney Disease: known knowns and known unknowns. Kidney Int. 105, 684–701 (2024).
Google Scholar
Kidney Disease: Improving Global Outcomes (KDIGO) CKD Work Group. KDIGO 2012 clinical practice guideline for the evaluation and management of chronic kidney disease. Kidney Int. Suppl. 3, 1–150 (2013).
Feldman, H. I. et al. The chronic renal insufficiency cohort (CRIC) study: design and methods. J. Am. Soc. Nephrol. 14, S148–S153 (2003).
Google Scholar
Stengel, B. et al. The French Chronic Kidney Disease-Renal Epidemiology and Information Network (CKD-REIN) cohort study. Nephrol. Dial. Transpl. 29, 1500–1507 (2014).
Google Scholar
Eckardt, K.-U. et al. The German Chronic Kidney Disease (GCKD) study: design and methods. Nephrol. Dial. Transplant. 27, 1454–1460 (2012).
Google Scholar
Hoshino, J. et al. A nationwide prospective cohort study of patients with advanced chronic kidney disease in Japan: the reach-J CKD cohort study. Clin. Exp. Nephrol. 22, 309–317 (2018).
Google Scholar
Dienemann, T. et al. International network of chronic kidney disease cohort studies (iNET-CKD): a global network of chronic kidney disease cohorts. BMC Nephrol. 17, 121 (2016).
Google Scholar
Jager, K. J. et al. The EQUAL study: a European study in chronic kidney disease stage 4 patients. Nephrol. Dial. Transpl. 27, iii27–31 (2012).
Google Scholar
GBD Chronic Kidney Disease Collaboration. Global, regional, and national burden of chronic kidney disease, 1990–2017: a systematic analysis for the global burden of disease study 2017. Lancet 395, 709–733 (2020).
Google Scholar
Bello, A. K. et al. Status of care for end stage kidney disease in countries and regions worldwide: international cross sectional survey. BMJ 367, l5873 (2019).
Google Scholar
van Rijn, M. H. C., de Pinho, N. A., Wetzels, J. F., van den Brand, J. A. J. G. & Stengel, B. Worldwide disparity in the relation between CKD prevalence and kidney failure risk. Kidney Int. Rep. 5, 2284–2291 (2020).
Google Scholar
Yeung, E. et al. Current status of health systems financing and oversight for end-stage kidney disease care: a cross-sectional global survey. BMJ Open. 11, e047245 (2021).
Google Scholar
Pinho et al. Understanding international variations in kidney failure incidence and initiation of replacement therapy. Kidney Int. Rep. 7, 2364–2375 (2022).
Google Scholar
Neuen, B. L. et al. National health policies and strategies for addressing chronic kidney disease: data from the International Society of Nephrology Global Kidney Health Atlas. PLoS Glob. Public Health 3, e0001467 (2023).
Google Scholar
Htay, H. et al. Global access of patients with kidney disease to health technologies and medications: findings from the global kidney health atlas project. Kidney Int. Suppl. 8, 64–73 (2018).
Google Scholar
Writing Group for the CKD Prognosis Consortium et al. Estimated glomerular filtration rate, albuminuria, and adverse outcomes. JAMA 330, 1266–1277 (2023).
Google Scholar
Kula, A. J., Prince, D. K., Katz, R. & Bansal, N. Mortality burden and life-years lost across the age spectrum for adults living with CKD. Kidney360 4, 615–621 (2023).
Google Scholar
Levey, A. S. et al. The definition, classification, and prognosis of chronic kidney disease: a KDIGO controversies conference report. Kidney Int. 80, 17–28 (2011).
Google Scholar
Hallan, S. I. et al. Screening strategies for chronic kidney disease in the general population: follow-up of cross sectional health survey. BMJ 333, 1047 (2006).
Google Scholar
Grams, M. E. et al. Predicting timing of clinical outcomes in patients with chronic kidney disease and severely decreased glomerular filtration rate. Kidney Int. 93, 1442–1451 (2018).
Google Scholar
Tonelli, M. et al. Risk of coronary events in people with chronic kidney disease compared with those with diabetes: a population-level cohort study. Lancet 380, 807–14 (2012).
Google Scholar
Tangri, N. et al. Multinational assessment of accuracy of equations for predicting risk of kidney failure: a meta-analysis. JAMA 315, 164–11 (2016).
Google Scholar
Bhandari, S., Mehta, S., Ives, N. & Cockwell, P. Utility of 2-year kidney failure risk equation for advanced chronic kidney disease: analysis from the STOP-ACEi trial. Nephrol. Dial. Transplant. 39, 884–887 (2023).
Google Scholar
Zacharias, H. U. et al. A predictive model for progression of CKD to kidney failure based on routine laboratory tests. Am. J. Kidney Dis. 79, 217–230.e1 (2021).
Google Scholar
Massy, Z. A. et al. Machine learning-based urine peptidome analysis to predict and understand mechanisms of progression to kidney failure. Kidney Int. Rep. 8, 544–555 (2023).
Google Scholar
Grams, M. E. et al. The kidney failure risk equation: evaluation of novel input variables including EGFR estimated using the CKD-EPI 2021 equation in 59 cohorts. J. Am. Soc. Nephrol. 34, 482–494 (2023).
Google Scholar
Ali, I., Donne, R. L. & Kalra, P. A. A validation study of the kidney failure risk equation in advanced chronic kidney disease according to disease aetiology with evaluation of discrimination, calibration and clinical utility. BMC Nephrol. 22, 194 (2021).
Google Scholar
Hundemer, G. L. et al. Performance of the kidney failure risk equation by disease etiology in advanced CKD. Clin. J. Am. Soc. Nephrol. 15, 1424–1432 (2020).
Google Scholar
Chu, C. D. et al. Utility of the kidney failure risk equation and estimated GFR for estimating time to kidney failure in advanced CKD. Am. J. Kidney Dis. 82, 386–394.e1 (2023).
Google Scholar
Inker, L. A. et al. A meta-analysis of GFR slope as a surrogate endpoint for kidney failure. Nat. Med. 29, 1867–1876 (2023).
Google Scholar
Weiner, D. E. et al. The Framingham predictive instrument in chronic kidney disease. J. Am. Coll. Cardiol. 50, 217–224 (2007).
Google Scholar
Matsushita, K., Ballew, S. H. & Coresh, J. Cardiovascular risk prediction in people with chronic kidney disease. Curr. Opin. Nephrol. Hypertens. 25, 518–523 (2016).
Google Scholar
Matsushita, K. et al. Estimated glomerular filtration rate and albuminuria for prediction of cardiovascular outcomes: a collaborative meta-analysis of individual participant data. Lancet Diabetes Endocrinol. 3, 514–525 (2015).
Google Scholar
Matsushita, K. et al. Incorporating kidney disease measures into cardiovascular risk prediction: development and validation in 9 million adults from 72 datasets. Eclinicalmedicine 27, 100552 (2020).
Google Scholar
Shlipak, M. G. et al. Cardiovascular mortality risk in chronic kidney disease: comparison of traditional and novel risk factors. JAMA 293, 1737–1745 (2005).
Google Scholar
Bundy, J. D. et al. Risk prediction models for atherosclerotic cardiovascular disease in patients with chronic kidney disease: the CRIC study. J. Am. Soc. Nephrol. 33, 601–611 (2022).
Google Scholar
Massy, Z. A. & Drueke, T. B. Combination of cardiovascular, kidney, and metabolic diseases in a syndrome named cardiovascular-kidney-metabolic, with new risk prediction equations. Kidney Int. Rep. 9, 2608–2618 (2024).
Google Scholar
Drüeke, T. B. & Massy, Z. A. Atherosclerosis in CKD: differences from the general population. Nat. Rev. Nephrol. 6, 723–735 (2010).
Google Scholar
Lees, J. S. et al. Glomerular filtration rate by differing measures, albuminuria and prediction of cardiovascular disease, mortality and end-stage kidney disease. Nat. Med. 25, 1753–1760 (2019).
Google Scholar
Lees, J. S. et al. Assessment of cystatin C level for risk stratification in adults with chronic kidney disease. JAMA Netw. Open 5, e2238300 (2022).
Google Scholar
Kalantar-Zadeh, K. et al. Patient-centred approaches for the management of unpleasant symptoms in kidney disease. Nat. Rev. Nephrol. 18, 185–198 (2022).
Google Scholar
Speyer, E. et al. Symptom burden and its impact on quality of life in patients with moderate to severe CKD: the international chronic kidney disease outcomes and practice patterns study (CKDopps). Am. J. Kidney Dis. 84, 696–707.e1 (2024).
Google Scholar
Mallamaci, F., Pisano, A. & Tripepi, G. Physical activity in chronic kidney disease and the EXerCise introduction to enhance trial. Nephrol. Dial. Transplant. 35, ii18–ii22 (2020).
Google Scholar
Curtis, F. et al. Lifestyle interventions delivered by eHealth in chronic kidney disease: a scoping review. PLoS ONE 19, e0297107 (2024).
Google Scholar
Greenwood, S. A. et al. Evaluating the effect of a digital health intervention to enhance physical activity in people with chronic kidney disease (Kidney BEAM): a multicentre, randomised controlled trial in the UK. Lancet Digit. Health 6, e23–e32 (2024).
Google Scholar
Greenwood, S. A. et al. Kidney beam — a cost-effective digital intervention to improve mental health. Kidney Int. Rep. 9, 3204–3217 (2024).
Google Scholar
Tantisattamo, E. et al. Novel approaches to sarcopenic obesity and weight management before and after kidney transplantation. Curr. Opin. Nephrol. Hypertens. 30, 14–26 (2021).
Google Scholar
Martins, P. et al. Association between physical activity and mortality in end-stage kidney disease: a systematic review of observational studies. BMC Nephrol. 22, 227 (2021).
Google Scholar
Zoccali, C., Manfredini, F., Kanbay, M. & Mallamaci, F. Intradialysis exercise in hemodialysis patients: effective but complex and costly. Nephrol. Dial. Transplant. 39, 7–9 (2023).
Google Scholar
American Diabetes Association Professional Practice Committee for Diabetes. 9. Pharmacologic approaches to glycemic treatment: standards of care in diabetes — 2026. Diabetes Care 49, S183–S215 (2025).
Google Scholar
Kidney Disease: Improving Global Outcomes (KDIGO) Diabetes Work Group. KDIGO 2020 clinical practice guideline for diabetes management in chronic kidney disease. Kidney Int. 98, S1–S115 (2020).
Google Scholar
Herrington, W. G. & Haynes, R. Diabetic kidney disease — semaglutide flows into the mainstream. N. Engl. J. Med. 391, 178–179 (2024).
Google Scholar
de Boer, I. H. et al. Diabetes management in chronic kidney disease: a consensus report by the American Diabetes Association (ADA) and Kidney Disease: Improving Global Outcomes (KDIGO). Kidney Int. 102, 974–989 (2022).
Google Scholar
ElSayed, N. A. et al. Summary of revisions: standards of care in diabetes — 2023. Diabetes Care 46, S5–S9 (2022).
Google Scholar
Bakris, G. L. & Molitch, M. Microalbuminuria as a risk predictor in diabetes: the continuing saga. Diabetes Care 37, 867–875 (2014).
Google Scholar
Kalantar-Zadeh, K. & Fouque, D. Nutritional management of chronic kidney disease. N. Engl. J. Med. 377, 1765–1776 (2017).
Google Scholar
Faye, M. et al. Five-year symptom trajectories in nondialysis-dependent CKD patients. Clin. J. Am. Soc. Nephrol. 17, 1588–1597 (2022).
Google Scholar
Kelly, J. T. et al. Healthy dietary patterns and risk of mortality and ESRD in CKD: a meta-analysis of cohort studies. Clin. J. Am. Soc. Nephrol. 12, 272–279 (2017).
Google Scholar
Burnier, M. Sodium intake and progression of chronic kidney disease — has the time finally come to do the impossible: a prospective randomized controlled trial? Nephrol. Dial. Transplant. 36, 381–384 (2020).
Google Scholar
Borrelli, S. et al. Sodium intake and chronic kidney disease. Int. J. Mol. Sci. 21, 4744 (2020).
Google Scholar
Tomson, C. R. V. Advising dialysis patients to restrict fluid intake without restricting sodium intake is not based on evidence and is a waste of time. Nephrol. Dial. Transplant. 16, 1538–1542 (2001).
Google Scholar
Afsar, B., Afsar, R. E., Caliskan, Y. & Lentine, K. L. A holistic review of sodium intake in kidney transplant patients: more questions than answers. Transplant. Rev. 38, 100859 (2024).
Google Scholar
Ikizler, T. A. et al. KDOQI clinical practice guideline for nutrition in CKD: 2020 update. Am. J. Kidney Dis. 76, S1–S107 (2020).
Google Scholar
Fouque, D. et al. Insulin-like growth factor-1 and its binding proteins during a low-protein diet in chronic renal failure. J. Am. Soc. Nephrol. 6, 1427–1433 (1995).
Google Scholar
Wang, A. Y.-M. et al. Precision medicine for nutritional management in end-stage kidney disease and transition to dialysis. Semin. Nephrol. 38, 383–396 (2018).
Google Scholar
Carrero, J. J. et al. Plant-based diets to manage the risks and complications of chronic kidney disease. Nat. Rev. Nephrol. 16, 1–18 (2020).
Google Scholar
Bakis, H., Chauveau, P., Combe, C. & Pfirmann, P. Mediterranean diet for cardiovascular risk reduction in chronic kidney disease. Adv. Kidney Dis. Health 30, 496–501 (2023).
Google Scholar
Joshi, S., McMacken, M. & Kalantar-Zadeh, K. Plant-based diets for kidney disease: a guide for clinicians. Am. J. Kidney Dis. 77, 287–296 (2021).
Google Scholar
Goraya, N. & Wesson, D. E. Plant-based diets across the spectrum of kidney disease. Clin. J. Am. Soc. Nephrol. 20, 1142–1149 (2025).
Google Scholar
Sumida, K. et al. Constipation and Incident CKD. J. Am. Soc. Nephrol. 28, 1248–1258 (2017).
Google Scholar
Fouque, D., Mafra, D. & Bellizzi, V. Dietary protein intake in CKD: quantity and quality. Clin. J. Am. Soc. Nephrol. (2025).
Google Scholar
Wang, A. Y.-M. et al. Assessing global kidney nutrition care. Clin. J. Am. Soc. Nephrol. 17, 38–52 (2022).
Google Scholar
St-Jules, D. E. & Fouque, D. Etiology-based dietary approach for managing hyperkalemia in people with chronic kidney disease. Nutr. Rev. 80, 2198–2205 (2022).
Google Scholar
Weir, M. R. et al. Patiromer in patients with kidney disease and hyperkalemia receiving RAAS inhibitors. N. Engl. J. Med. 372, 211–221 (2014).
Google Scholar
Agarwal, R. et al. Patiromer versus placebo to enable spironolactone use in patients with resistant hypertension and chronic kidney disease (AMBER): a phase 2, randomised, double-blind, placebo-controlled trial. Lancet 394, 1540–1550 (2019).
Google Scholar
St-Jules, D. E., Clegg, D. J., Palmer, B. F. & Carrero, J.-J. Can novel potassium binders liberate people with chronic kidney disease from the low-potassium diet? Clin. J. Am. Soc. Nephrol. 17, 467–472 (2022).
Google Scholar
Packer, M. Potassium binders for patients with heart failure? The real enlightenment of the DIAMOND trial. Eur. Heart J. 43, 4374–4377 (2022).
Google Scholar
Sumida, K. et al. Laxative use and risk of dyskalemia in patients with advanced CKD transitioning to dialysis. J. Am. Soc. Nephrol. 32, 950–959 (2021).
Google Scholar
Levin, A. et al. Prevalence of abnormal serum vitamin D, PTH, calcium, and phosphorus in patients with chronic kidney disease: results of the study to evaluate early kidney disease. Kidney Int. 71, 31–38 (2007).
Google Scholar
Moranne, O. et al. Timing of onset of CKD-related metabolic complications. J. Am. Soc. Nephrol. 20, 164–171 (2009).
Google Scholar
Zoccali, C. et al. The systemic nature of CKD. Nat. Rev. Nephrol. 13, 1–15 (2017).
Google Scholar
Costes-Albrespic, M. et al. Antihypertensive treatment patterns in CKD stages 3 and 4: the CKD-REIN Cohort Study. Kidney Med. 6, 100912 (2024).
Google Scholar
Pinho et al. Considerable international variation exists in blood pressure control and antihypertensive prescription patterns in chronic kidney disease. Kidney Int. 96, 983–994 (2019).
Google Scholar
Weir, M. R. et al. Use of renin-angiotensin system blockade in advanced CKD: an NKF-KDOQI controversies report. Am. J. Kidney Dis. 72, 873–884 (2018).
Google Scholar
Ingelfinger, J. R. Discontinuation of RAS inhibitors in advanced CKD — has equipoise occurred? N. Engl. J. Med. 387, 2083–2084 (2022).
Google Scholar
Cheung, A. K. et al. Executive summary of the KDIGO 2021 clinical practice guideline for the management of blood pressure in chronic kidney disease. Kidney Int. 99, 559–569 (2021).
Google Scholar
Pugh, D., Gallacher, P. J. & Dhaun, N. Management of hypertension in chronic kidney disease. Drugs 79, 365–379 (2019).
Google Scholar
Pecoits-Filho, R. et al. Prescription of renin-angiotensin-aldosterone system inhibitors (RAASi) and its determinants in patients with advanced CKD under nephrologist care. J. Clin. Hypertens. 21, 337–11 (2019).
Google Scholar
Bhandari, S. et al. Renin–angiotensin system inhibition in advanced chronic kidney disease. N. Engl. J. Med. 387, 2021–2032 (2022).
Google Scholar
Fu, E. L. et al. Stopping renin-angiotensin system inhibitors in patients with advanced CKD and risk of adverse outcomes: a nationwide study. J. Am. Soc. Nephrol. 32, 424–435 (2021).
Google Scholar
Karaboyas, A. et al. DOPPS data suggest a possible survival benefit of renin angiotensin-aldosterone system inhibitors and other antihypertensive medications for hemodialysis patients. Kidney Int. 94, 589–598 (2018).
Google Scholar
Bushinsky, D. A. et al. Patiromer treatment in patients with CKD, hyperkalemia, and hyperphosphatemia: a post hoc analysis of 3 clinical trials. Am. J. Kidney Dis. 82, 97–104 (2023).
Google Scholar
Shi, Q. et al. Benefits and harms of drug treatment for type 2 diabetes: systematic review and network meta-analysis of randomised controlled trials. BMJ. 381, e074068 (2023).
Google Scholar
Rangaswami, J. & Mathew, R. O. Reducing kidney disease burden in type 2 diabetes with SGLT2 inhibitors: shifting the goalposts upstream. Clin. J. Am. Soc. Nephrol. 18, 1119–1121 (2023).
Google Scholar
Braunwald, E. Gliflozins in the management of cardiovascular disease. N. Engl. J. Med. 386, 2024–2034 (2022).
Google Scholar
Zannad, F. et al. SGLT2 inhibitors in patients with heart failure with reduced ejection fraction: a meta-analysis of the EMPEROR-Reduced and DAPA-HF trials. Lancet 396, 819–829 (2020).
Google Scholar
Wheeler, D. C. et al. Effects of dapagliflozin on major adverse kidney and cardiovascular events in patients with diabetic and non-diabetic chronic kidney disease: a prespecified analysis from the DAPA-CKD trial. Lancet Diabetes Endocrinol. 9, 22–31 (2021).
Google Scholar
Heerspink, H. J. L. et al. Dapagliflozin in patients with chronic kidney disease. N. Engl. J. Med. 383, 1436–1446 (2020).
Google Scholar
EMPA-KIDNEY Collaborative Group. et al. Long-term effects of empagliflozin in patients with chronic kidney disease. N. Engl. J. Med. 392, 777–787 (2025).
Google Scholar
The EMPA-KIDNEY Collaborative Group. et al. Empagliflozin in patients with chronic kidney disease. N. Engl. J. Med. 388, 117–127 (2022).
Google Scholar
Wheeler, D. C. et al. A pre-specified analysis of the DAPA-CKD trial demonstrates the effects of dapagliflozin on major adverse kidney events in patients with IgA nephropathy. Kidney Int. 100, 215–224 (2021).
Google Scholar
Kidney Disease: Improving Global Outcomes (KDIGO) Diabetes Work Group KDIGO 2022 clinical practice guideline for diabetes management in chronic kidney disease. Kidney Int. 102, S1–S127 (2022).
Google Scholar
Singh, T., Li, T., Mandebrot, D., Astor, B. C. & Mehr, A. P. Prescribing patterns for sodium-glucose Co-transporter 2 Inhibitors (SGLT2i): a survey of nephrologists. Kidney Int. Rep. 8, 1669–1671 (2023).
Google Scholar
Leaf, D. E. & Bansal, N. Another win for SGLT2 inhibitors in chronic kidney disease. N. Engl. J. Med. 392, 822–823 (2025).
Google Scholar
Heerspink, H. J. L., Berger, S., Gansevoort, R. T. on behalf of the Renal Life Cycle Trial Investigators. Will SGLT2 inhibitors be effective and safe in patients with severe CKD, dialysis, or kidney transplantation. Clin. J. Am. Soc. Nephrol. 18, 1500–1502 (2023).
Google Scholar
Yen, F.-S. et al. Sodium-glucose cotransporter-2 inhibitors and the risk for dialysis and cardiovascular disease in patients with stage 5 chronic kidney disease. Ann. Intern. Med. 177, 693–700 (2024).
Google Scholar
Cohen, T. D. et al. Safety of sodium-glucose cotransporter 2 inhibitors in kidney transplant recipients with diabetes mellitus. Diabetes Metab. 51, 101627 (2025).
Google Scholar
Holliday, M. W., Frost, L. & Navaneethan, S. D. Emerging evidence for glucagon-like peptide-1 agonists in slowing chronic kidney disease progression. Curr. Opin. Nephrol. Hypertens. 33, 331–336 (2024).
Google Scholar
Perkovic, V. et al. Effects of semaglutide on chronic kidney disease in patients with type 2 diabetes. N. Engl. J. Med. 391, 109–121 (2024).
Google Scholar
Apperloo, E. M. et al. Semaglutide in patients with overweight or obesity and chronic kidney disease without diabetes: a randomized double-blind placebo-controlled clinical trial. Nat. Med. 31, 278–285 (2024).
Google Scholar
Zelada, H. et al. Efficacy, tolerability, and safety of glucagon-like peptide 1 receptor agonists (GLP1-RA) in kidney transplant recipients with diabetes. Clin. Transplant. 39, e70144 (2025).
Google Scholar
Cohen, T. D. et al. Glucagon-like peptide 1 receptor agonists and renal outcomes in kidney transplant recipients with diabetes mellitus. Diabetes Metab. 51, 101624 (2025).
Google Scholar
Bellos, I., Lagiou, P., Benetou, V. & Marinaki, S. Safety and efficacy of sodium-glucose transport protein 2 inhibitors and glucagon-like peptide-1 receptor agonists in diabetic kidney transplant recipients: synthesis of evidence. J. Clin. Med. 13, 6181 (2024).
Google Scholar
Lai, H.-W., See, C. Y., Chen, J.-Y. & Wu, V.-C. Mortality and cardiovascular events in diabetes mellitus patients at dialysis initiation treated with glucagon-like peptide-1 receptor agonists. Cardiovasc. Diabetol. 23, 277 (2024).
Google Scholar
Thomas, A. M., Lamb, K. & Howard, O. Glucagon-like peptide-1 receptor agonists use for type 2 diabetes mellitus in end-stage renal disease. J. Am. Pharm. Assoc. 63, 1612–1616 (2023).
Google Scholar
Orandi, B. J. et al. GLP-1 receptor agonist outcomes, safety, and body mass index change in a national cohort of patients on dialysis. Clin. J. Am. Soc. Nephrol. 20, 1100–1110 (2025).
Google Scholar
Agarwal, R. et al. Chlorthalidone for hypertension in advanced chronic kidney disease. N. Engl. J. Med. 385, 2507–2519 (2021).
Google Scholar
Agarwal, R., Sinha, A. D. & Tu, W. Mechanisms of antihypertensive effect of chlorthalidone in advanced chronic kidney disease. Clin. J. Am. Soc. Nephrol. 19, 1025–1032 (2024).
Google Scholar
Jafar, T. H. & Feng, L. Understanding the BP-lowering mechanism of chlorthalidone in advanced kidney disease. Clin. J. Am. Soc. Nephrol. 19, 949–951 (2024).
Google Scholar
Agarwal, R., Verma, A. & Georgianos, P. I. Diuretics in patients with chronic kidney disease. Nat. Rev. Nephrol. 21, 264–278 (2025).
Google Scholar
Faucon, A.-L. et al. A nationwide cohort study comparing the effectiveness of diuretics and calcium channel blockers on top of renin-angiotensin system inhibitors on chronic kidney disease progression and mortality. Kidney Int. 104, 542–551 (2023).
Google Scholar
Tabibzadeh, N. et al. Diuretic prescriptions in the first year of haemodialysis: international practice patterns and associations with outcomes. Clin. Kidney J. 17, sfae141 (2024).
Google Scholar
Sarafidis, P. et al. Outcomes with finerenone in participants with stage 4 CKD and type 2 diabetes. Clin. J. Am. Soc. Nephrol. 18, 602–612 (2023).
Google Scholar
Massy, Z. A. et al. Achievement of low-density lipoprotein cholesterol targets in CKD. Kidney Int. Rep. 4, 1546–1554 (2019).
Google Scholar
Massy, Z. A. et al. Is a treat-to-target approach to lipid-lowering therapy appropriate in patients with chronic kidney disease? A prospective French cohort study. J. Nephrol 34, 1467–1477 (2021).
Google Scholar
KDIGO clinical practice guideline for lipid management in chronic kidney disease. Kidney Int. Suppl. 3, 1–56 (2013).
Massy, Z. A. et al. Association of serum phosphate with efficacy of statin therapy in hemodialysis patients. Clin. J. Am. Soc. Nephrol. 17, 546–554 (2022).
Google Scholar
Baigent, C. et al. The effects of lowering LDL cholesterol with simvastatin plus ezetimibe in patients with chronic kidney disease (Study of Heart and Renal Protection): a randomised placebo-controlled trial. Lancet 377, 2181–2192 (2011).
Google Scholar
Canney, M. et al. Regional variation in hemoglobin distribution among individuals with CKD: the ISN International Network of CKD Cohorts. Kidney Int. Rep. 8, 2056–2067 (2023).
Google Scholar
KDIGO clinical practice guideline for anemia in chronic kidney disease. Kidney Int. Suppl. 2, 179 (2012).
Kliger, A. S. et al. KDOQI US commentary on the 2012 KDIGO clinical practice guideline for anemia in CKD. Am. J. Kidney Dis. 62, 849–859 (2013).
Google Scholar
Locatelli, F. et al. Kidney disease: improving global outcomes guidelines on anaemia management in chronic kidney disease: a European renal best practice position statement. Nephrol. Dial. Transplant. 28, 1346–1359 (2013).
Google Scholar
Bhandari, S. et al. UK Kidney Association clinical practice guideline: update of anaemia of chronic kidney disease. BMC Nephrol. 26, 193 (2025).
Google Scholar
Lopes, M. B. et al. A real-world longitudinal study of anemia management in non-dialysis-dependent chronic kidney disease patients: a multinational analysis of CKDopps. Sci. Rep. 11, 1784 (2021).
Google Scholar
Guedes, M. et al. Serum biomarkers of iron stores are associated with increased risk of all-cause mortality and cardiovascular events in nondialysis CKD patients, with or without anemia. J. Am. Soc. Nephrol. 32, 2020–2030 (2021).
Google Scholar
Gall, L. L. et al. Haemoglobin trajectories in chronic kidney disease and risk of major adverse cardiovascular events. Nephrol. Dial. Transplant. 39, 669–682 (2023).
Google Scholar
Locatelli, F. & Vecchio, L. D. Hypoxia-inducible factor–prolyl hydroxyl domain inhibitors: from theoretical superiority to clinical noninferiority compared with current ESAs? J. Am. Soc. Nephrol. 33, 1966–1979 (2022).
Google Scholar
KDIGO 2017 clinical practice guideline update for the diagnosis, evaluation, prevention, and treatment of chronic kidney disease–mineral and bone disorder (CKD-MBD). Kidney Int. Suppl. 7, 1–59 (2017).
Liabeuf, S. et al. International variation in the management of mineral bone disorder in patients with chronic kidney disease: results from CKDopps. Bone 129, 115058 (2019).
Google Scholar
Sweiss, H. et al. Safety and efficacy of sodium-glucose cotransporter-2 inhibitors in solid organ transplant recipients. Prog. Transpl. 33, 261–265 (2023).
Google Scholar
US National Library of Medicine. ClinicalTrials.gov (2025).
Karaboyas, A. et al. Estimating the fraction of first-year hemodialysis deaths attributable to potentially modifiable risk factors: results from the DOPPS. Clin. Epidemiol. 12, 51–60 (2020).
Google Scholar
Liu, Y., Ma, X., Zheng, J., Jia, J. & Yan, T. Effects of angiotensin-converting enzyme inhibitors and angiotensin receptor blockers on cardiovascular events and residual renal function in dialysis patients: a meta-analysis of randomised controlled trials. BMC Nephrol. 18, 206 (2017).
Google Scholar
Barreto, J. et al. Pharmacokinetic properties of dapagliflozin in hemodialysis and peritoneal dialysis patients. Clin. J. Am. Soc. Nephrol. 18, 1051–1058 (2023).
Google Scholar
Walsh, M. et al. Spironolactone versus placebo in patients undergoing maintenance dialysis (ACHIEVE): an international, parallel-group, randomised controlled trial. Lancet 406, 695–704 (2025).
Google Scholar
Rossignol, P. et al. Spironolactone in patients on chronic haemodialysis at high risk of adverse cardiovascular outcomes (ALCHEMIST): a multicentre, double-blind, randomised, placebo-controlled trial and updated meta-analysis. Lancet 406, 705–718 (2025).
Google Scholar
Abramowicz, D. et al. Does pre-emptive transplantation versus post start of dialysis transplantation with a kidney from a living donor improve outcomes after transplantation? A systematic literature review and position statement by the Descartes working group and ERBP. Nephrol. Dial. Transplant. 31, 691–697 (2016).
Google Scholar
Meier-Kriesche, H.-U. et al. Effect of waiting time on renal transplant outcome. Kidney Int. 58, 1311–1317 (2000).
Google Scholar
Mange, K. C., Joffe, M. M. & Feldman, H. I. Effect of the use or nonuse of long-term dialysis on the subsequent survival of renal transplants from living donors. N. Engl. J. Med. 344, 726–731 (2001).
Google Scholar
Prezelin-Reydit, M. et al. Prolonged dialysis duration is associated with graft failure and mortality after kidney transplantation: results from the French transplant database. Nephrol. Dial. Transpl. 34, 538–545 (2018).
Google Scholar
Goto, N. et al. Association of dialysis duration with outcomes after transplantation in a Japanese cohort. Clin. J. Am. Soc. Nephrol. 11, 497–504 (2016).
Google Scholar
Strohmaier, S. et al. Survival benefit of first single-organ deceased donor kidney transplantation compared with long-term dialysis across ages in transplant-eligible patients with kidney failure. JAMA Netw. Open 5, e2234971 (2022).
Google Scholar
McCormick, F., Held, P. J., Chertow, G. M., Peters, T. G. & Roberts, J. P. Removing disincentives to kidney donation: a quantitative analysis. J. Am. Soc. Nephrol. 30, 1349–1357 (2019).
Google Scholar
Held, P. J., McCormick, F., Ojo, A. & Roberts, J. P. A cost-benefit analysis of government compensation of kidney donors. Am. J. Transpl. 16, 877–885 (2015).
Google Scholar
REIN annual report 2021: summary. (2023).
Gadelkareem, R. A. et al. Preemptive living donor kidney transplantation: access, fate, and review of the status in Egypt. World J. Nephrol. 12, 40–55 (2023).
Google Scholar
Shah, D. S. Insights from Nepal into implementing transplantation programmes in low-resource settings. Nat. Rev. Nephrol. 21, 812 (2025).
Google Scholar
Cheddani, L. et al. Higher mortality risk among kidney transplant recipients than among estimated glomerular filtration rate-matched patients with CKD — preliminary results. Nephrol. Dial. Transplant. 36, 176–184 (2020).
Google Scholar
Wolfe, R. A. et al. Comparison of mortality in all patients on dialysis, patients on dialysis awaiting transplantation, and recipients of a first cadaveric transplant. N. Engl. J. Med. 341, 1725–1730 (1999).
Google Scholar
Gander, J. C. et al. Association between dialysis facility ownership and access to kidney transplantation. JAMA 322, 957 (2019).
Google Scholar
Chan, C. T. et al. Dialysis initiation, modality choice, access, and prescription: conclusions from a Kidney Disease: Improving Global Outcomes (KDIGO) controversies conference. Kidney Int. 96, 37–47 (2019).
Google Scholar
Cheetham, M. S. et al. Home versus in-centre haemodialysis for people with kidney failure. Cochrane Database Syst. Rev. 2024, CD009535 (2024).
Fages, V. et al. Urgent-start dialysis in patients referred early to a nephrologist — the CKD-REIN prospective cohort study. Nephrol. Dial. Transpl. 36, 1500–1510 (2021).
Google Scholar
Robinson, B. M. et al. Worldwide, mortality risk is high soon after initiation of hemodialysis. Kidney Int. 85, 158–165 (2014).
Google Scholar
Lok, C. E. et al. KDOQI clinical practice guideline for vascular access: 2019 update. Am. J. Kidney Dis. 75, S1–S164 (2020).
Google Scholar
Pisoni, R. L. et al. International comparisons of native arteriovenous fistula patency and time to becoming catheter-free: findings from the dialysis outcomes and practice patterns study (DOPPS). Am. J. Kidney Dis. 77, 245–254 (2021).
Google Scholar
Pisoni, R. L. et al. Facility hemodialysis vascular access use and mortality in countries participating in DOPPS: an instrumental variable analysis. Am. J. Kidney Dis. 53, 475–491 (2009).
Google Scholar
Faye, M. et al. Vascular access in Senegalese patients starting chronic haemodialysis. Afr. J. Nephrol. 26, 3–8, (2023).
Google Scholar
Couchoud, C. et al. Dialysis modality choice in diabetic patients with end-stage kidney disease: a systematic review of the available evidence. Nephrol. Dial. Transpl. 30, 310–320 (2015).
Google Scholar
Combe, C., Rigothier, C. & Chauveau, P. Evidence-based choice of dialysis technique in diabetics with end-stage kidney disease: half a loaf is better than no bread. Nephrol. Dial. Transpl. 30, 160–162 (2015).
Google Scholar
Montez-Rath, M. E. et al. Effect of starting dialysis versus continuing medical management on survival and home time in older adults with kidney failure: a target trial emulation study. Ann. Intern. Med. 177, 1233–1243 (2024).
Google Scholar
Jaques, D. A. et al. Outcomes of incident patients treated with incremental haemodialysis as compared with standard haemodialysis and peritoneal dialysis. Nephrol. Dial. Transpl. 37, 2514–2521 (2022).
Google Scholar
Wanner, C., Lopau, K. & Haberstroh, H. The safety and feasibility of incremental dialysis must be proven before its widespread use. Kidney Int. 101, 468–471 (2022).
Google Scholar
Murea, M. et al. From niche to norm: a multi-action plan to close gaps and mainstream incremental hemodialysis. Kidney Int. 108, 201–213 (2025).
Google Scholar
Elliott, M. J. et al. Patient and clinician perspectives on shared decision making in vascular access selection: a qualitative study. Am. J. Kidney Dis. 81, 48–58.e1 (2023).
Google Scholar
Pisoni, R. L., Zepel, L., Port, F. K. & Robinson, B. M. Trends in US vascular access use, patient preferences, and related practices: an update from the US DOPPS practice monitor with international comparisons. Am. J. Kidney Dis. 65, 905–915 (2015).
Google Scholar
Hecking, M. et al. Sex-specific differences in mortality and incident dialysis in the chronic kidney disease outcomes and practice patterns study. Kidney Int. Rep. 7, 410–423 (2021).
Google Scholar
de Pinho, N. A. et al. Predictors of nonfunctional arteriovenous access at hemodialysis initiation and timing of access creation: a registry-based study. PLoS ONE 12, e0181254 (2017).
Google Scholar
Griva, K. et al. Patient-related barriers to timely dialysis access preparation: a qualitative study of the perspectives of patients, family members, and health care providers. Kidney Med. 2, 29–41 (2020).
Google Scholar
Flythe, J. E. et al. Targeting patient and health system barriers to improve rates of hemodialysis initiation with an arteriovenous access. Kidney360 2, 708–720 (2021).
Google Scholar
Lopez-Vargas, P. A. et al. Barriers to timely arteriovenous fistula creation: a study of providers and patients. Am. J. Kidney Dis. 57, 873–882 (2011).
Google Scholar
Tabcheh, A.-H. et al. Arteriovenous access creation and eGFR decline in patients with CKD. J. Am. Soc. Nephrol. 35, 1570–1573 (2024).
Google Scholar
Brown, E. A. et al. International Society for Peritoneal Dialysis practice recommendations: prescribing high-quality goal-directed peritoneal dialysis. Perit. Dial. Int. 40, 244–253 (2020).
Google Scholar
Davison, S. N. et al. Executive summary of the KDIGO controversies conference on supportive care in chronic kidney disease: developing a roadmap to improving quality care. Kidney Int. 88, 447–459 (2015).
Google Scholar
Davison, S. N. et al. Conservative kidney management and kidney supportive care: core components of integrated care for people with kidney failure. Kidney Int. 105, 35–45 (2024).
Google Scholar
McMahan, R. D. & Sudore, R. L. Making advance care planning easier for adults with kidney disease and their clinicians. Nat. Rev. Nephrol. 20, 564–565 (2024).
Google Scholar
Hamroun, A., Glowacki, F. & Frimat, L. Comprehensive conservative care: what doctors say, what patients hear. Nephrol. Dial. Transpl. 38, 2428–2443 (2023).
Google Scholar
Ladin, K. et al. Characterizing approaches to dialysis decision making with older adults: a qualitative study of nephrologists. Clin. J. Am. Soc. Nephrol. 13, 1188–1196 (2018).
Google Scholar
Hounkpatin, H. O. et al. Patients’ and kidney care team’s perspectives of treatment burden and capacity in older people with chronic kidney disease: a qualitative study. BMJ Open. 10, e042548 (2020).
Google Scholar
Hamroun, A. et al. Barriers to conservative care from patients’ and nephrologists’ perspectives: the CKD-REIN study. Nephrol. Dial. Transpl. 37, 2438–2448 (2022).
Google Scholar
Morton, R. L. et al. Conservative management and end-of-life care in an Australian cohort with ESRD. Clin. J. Am. Soc. Nephrol. 11, 2195–2203 (2016).
Google Scholar
Jain, G. & Weiner, D. E. Value-based care in nephrology: the kidney care choices model and other reforms. (2021).
Centers for Medicare & Medicaid Services. ESRD treatment choices (ETC) model. (2025).
Lin, E., Dave, G. & Kshirsagar, A. V. The new kidney-focused companies: a privatized approach to value-based care and addressing social determinants of health. J. Am. Soc. Nephrol. 34, 17–20 (2023).
Google Scholar
Durand-Zaleski, I., Combe, C. & Lang, P. International study of health care organization and financing for end-stage renal disease in France. Int. J. Health Care Finance Econ. 7, 171–183 (2007).
Google Scholar
Vanholder, R. et al. Reimbursement of dialysis: a comparison of seven countries. J. Am. Soc. Nephrol. 23, 1291–1298 (2012).
Google Scholar
Arrêté du 25 septembre 2019 relatif aux forfaits alloués aux établissements de santé dans le cadre de la prise en charge de patients atteints de maladie rénale chronique en application de l’article L. 162-22-6-2 du code de la sécurité sociale. Journal Officiel de la République Française (2019).
Bello, A. et al. ISN — global kidney health atlas: a report by the International Society of Nephrology: an assessment of global kidney health care status focussing on capacity, availability, accessibility, affordability and outcomes of kidney disease. (2023).
Bello, A. K. et al. Global overview of health systems oversight and financing for kidney care. Kidney Int. Suppl. 8, 41–51 (2018).
Google Scholar
Okpechi, I. G. et al. Building optimal and sustainable kidney care in low resource settings: the role of healthcare systems. Nephrology 26, 948–960 (2021).
Google Scholar
link