The global epidemiology of acute kidney injury: challenges and opportunities
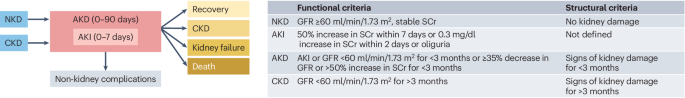
Ostermann, M. et al. Acute kidney injury. Lancet 405, 241–256 (2025).
Google Scholar
Chawla, L. S. et al. Association between AKI and long-term renal and cardiovascular outcomes in United States veterans. Clin. J. Am. Soc. Nephrol. 9, 448–456 (2014).
Google Scholar
Guthrie, G. et al. Developing an AKI consensus definition for database research: findings from a scoping review and expert opinion using a Delphi process. Am. J. Kidney Dis. 79, 488–496.e481 (2022).
Google Scholar
Lewington, A. J., Cerda, J. & Mehta, R. L. Raising awareness of acute kidney injury: a global perspective of a silent killer. Kidney Int. 84, 457–467 (2013).
Google Scholar
Nisula, S. et al. Incidence, risk factors and 90-day mortality of patients with acute kidney injury in Finnish intensive care units: the FINNAKI study. Intensive Care Med. 39, 420–428 (2013).
Google Scholar
Susantitaphong, P. et al. World incidence of AKI: a meta-analysis. Clin. J. Am. Soc. Nephrol. 8, 1482–1493 (2013).
Google Scholar
Verma, S. & Kellum, J. A. Defining acute kidney injury. Crit. Care Clin. 37, 251–266 (2021).
Google Scholar
Arias-Cabrales, C. et al. Short- and long-term outcomes after non-severe acute kidney injury. Clin. Exp. Nephrol. 22, 61–67 (2018).
Google Scholar
Hsu, C. Y. et al. Elevated BP after AKI. J. Am. Soc. Nephrol. 27, 914–923 (2016).
Google Scholar
Hoste, E. A. J. et al. Global epidemiology and outcomes of acute kidney injury. Nat. Rev. Nephrol. 14, 607–625 (2018).
Google Scholar
Acute Kidney Injury (AKI) TOOLKIT. International Society of Nephrology (2025).
Bellomo, R. et al. Acute renal failure — definition, outcome measures, animal models, fluid therapy and information technology needs: the second International Consensus Conference of the Acute Dialysis Quality Initiative (ADQI) group. Crit. Care 8, R204–R212 (2004).
Google Scholar
Mehta, R. L. et al. Acute kidney injury network: report of an initiative to improve outcomes in acute kidney injury. Crit. Care 11, R31 (2007).
Google Scholar
Hoste, E. A. & Kellum, J. A. Incidence, classification, and outcomes of acute kidney injury. Contrib. Nephrol. 156, 32–38 (2007).
Google Scholar
Mehta, R. L. et al. International Society of Nephrology’s 0by25 initiative for acute kidney injury (zero preventable deaths by 2025): a human rights case for nephrology. Lancet 385, 2616–2643 (2015).
Google Scholar
Kellum, J. A. et al. Acute kidney injury. Nat. Rev. Dis. Prim. 7, 52 (2021).
Google Scholar
Mehta, R. L. et al. Recognition and management of acute kidney injury in the International Society of Nephrology 0by25 Global Snapshot: a multinational cross-sectional study. Lancet 387, 2017–2025 (2016).
Google Scholar
Yang, L. et al. Acute kidney injury in China: a cross-sectional survey. Lancet 386, 1465–1471 (2015).
Google Scholar
Sohaney, R. et al. Trends in the incidence of acute kidney injury in a national cohort of US veterans. Am. J. Kidney Dis. 77, 300–302 (2021).
Google Scholar
Holmes, J., Donovan, K., Geen, J., Williams, J. & Phillips, A. O. Acute kidney injury demographics and outcomes: changes following introduction of electronic acute kidney injury alerts — an analysis of a national dataset. Nephrol. Dial. Transpl. 36, 1433–1439 (2021).
Google Scholar
Logan, R. et al. Assessing the accuracy of ICD-10 coding for measuring rates of and mortality from acute kidney injury and the impact of electronic alerts: an observational cohort study. Clin. Kidney J. 13, 1083–1090 (2020).
Google Scholar
Wilson, F. P. et al. A trial of in-hospital, electronic alerts for acute kidney injury: design and rationale. Clin. Trials 11, 521–529 (2014).
Google Scholar
Wilson, F. P. et al. Automated, electronic alerts for acute kidney injury: a single-blind, parallel-group, randomised controlled trial. Lancet 385, 1966–1974 (2015).
Google Scholar
Wilson, F. P. et al. A randomized clinical trial assessing the effect of automated medication-targeted alerts on acute kidney injury outcomes. Nat. Commun. 14, 2826 (2023).
Google Scholar
Zoccali, C. et al. Acute kidney injury, acute kidney disease, and chronic kidney disease: challenges and research perspectives. Nephrol. Dial. Transpl. (2025).
Sawhney, S. et al. Harmonization of epidemiology of acute kidney injury and acute kidney disease produces comparable findings across four geographic populations. Kidney Int. 101, 1271–1281 (2022).
Google Scholar
Lameire, N. H. et al. Harmonizing acute and chronic kidney disease definition and classification: report of a Kidney Disease: Improving Global Outcomes (KDIGO) consensus conference. Kidney Int. 100, 516–526 (2021).
Google Scholar
Macedo, E. et al. Recognition and management of acute kidney injury in children: the ISN 0by25 Global Snapshot study. PLoS ONE 13, e0196586 (2018).
Google Scholar
Macedo, E. et al. Recognition and management of community-acquired acute kidney injury in low-resource settings in the ISN 0by25 trial: a multi-country feasibility study. PLoS Med. 18, e1003408 (2021).
Google Scholar
James, M. T. et al. Incidence and prognosis of acute kidney diseases and disorders using an integrated approach to laboratory measurements in a universal health care system. JAMA Netw. Open 2, e191795 (2019).
Google Scholar
Sawhney, S. et al. Recovery of kidney function after acute kidney disease a multi-cohort analysis. Nephrol. Dial. Transpl. 39, 426–435 (2024).
Google Scholar
Horne, K. L. et al. A comprehensive description of kidney disease progression after acute kidney injury from a prospective, parallel-group cohort study. Kidney Int. 104, 1185–1193 (2023).
Google Scholar
Kashani, K., Rosner, M. H. & Ostermann, M. Creatinine: from physiology to clinical application. Eur. J. Intern. Med. 72, 9–14 (2020).
Google Scholar
Ostermann, M., Kashani, K. & Forni, L. G. The two sides of creatinine: both as bad as each other? J. Thorac. Dis. 8, E628–E630 (2016).
Google Scholar
Ostermann, M. et al. Recommendations on acute kidney injury biomarkers from the Acute Disease Quality Initiative Consensus Conference: a consensus statement. JAMA Netw. Open 3, e2019209 (2020).
Google Scholar
Ostermann, M. et al. Biomarkers in acute kidney injury. Ann. Intensive Care 14, 145 (2024).
Google Scholar
Haase, M., Kellum, J. A. & Ronco, C. Subclinical AKI — an emerging syndrome with important consequences. Nat. Rev. Nephrol. 8, 735–739 (2012).
Google Scholar
Ronco, C., Kellum, J. A. & Haase, M. Subclinical AKI is still AKI. Crit. Care 16, 313 (2012).
Google Scholar
Stanski, N., Menon, S., Goldstein, S. L. & Basu, R. K. Integration of urinary neutrophil gelatinase-associated lipocalin with serum creatinine delineates acute kidney injury phenotypes in critically ill children. J. Crit. Care 53, 1–7 (2019).
Google Scholar
Boutin, L., Chadjichristos, C., Mebazaa, A. & Depret, F. Postoperative subclinical AKI is frequent and is linked to a poor long-term prognosis in critically ill patients. Indian J. Anaesth. 69, 736–738 (2025).
Google Scholar
Zarbock, A. et al. Preventing acute kidney injury and its longer-term impact in the critically ill. Intensive Care Med. 51, 1331–1347 (2025).
Google Scholar
Marcello, M. et al. Subclinical AKI and clinical outcomes in elderly patients undergoing cardiac surgery: diagnostic utility of NGAL versus standard creatinine increase criteria. Cardiorenal Med. 12, 94–105 (2022).
Google Scholar
Moledina, D. G. et al. Performance of serum creatinine and kidney injury biomarkers for diagnosing histologic acute tubular injury. Am. J. Kidney Dis. 70, 807–816 (2017).
Google Scholar
de Boer, I. H. et al. Rationale and design of the Kidney Precision Medicine Project. Kidney Int. 99, 498–510 (2021).
Google Scholar
El-Achkar, T. M., Eadon, M. T., Kretzler, M., Himmelfarb, J. & Kidney Precision Medicine, P. Precision medicine in nephrology: an integrative framework of multidimensional data in the Kidney Precision Medicine Project. Am. J. Kidney Dis. 83, 402–410 (2024).
Google Scholar
Vaara, S. T. et al. Subphenotypes in acute kidney injury: a narrative review. Crit. Care 26, 251 (2022).
Google Scholar
Olowu, W. A. et al. Outcomes of acute kidney injury in children and adults in sub-Saharan Africa: a systematic review. Lancet Glob. Health 4, e242–e250 (2016).
Google Scholar
Jonny, J. et al. Incidence of acute kidney injury and use of renal replacement therapy in intensive care unit patients in Indonesia. BMC Nephrol. 21, 191 (2020).
Google Scholar
Lombardi, R. et al. Acute kidney injury in Latin America: a view on renal replacement therapy resources. Nephrol. Dial. Transpl. 29, 1369–1376 (2014).
Google Scholar
James, M. T., Bhatt, M., Pannu, N. & Tonelli, M. Long-term outcomes of acute kidney injury and strategies for improved care. Nat. Rev. Nephrol. 16, 193–205 (2020).
Google Scholar
Wainstein, M. et al. A global snapshot on health systems capacity for detection, monitoring, and management of acute kidney injury: a multinational study from the ISN-GKHA. PLOS Glob. Public Health 4, e0003823 (2024).
Google Scholar
Hoste, E. A. et al. Epidemiology of acute kidney injury in critically ill patients: the multinational AKI-EPI study. Intensive Care Med. 41, 1411–1423 (2015).
Google Scholar
Sileanu, F. E. et al. AKI in low-risk versus high-risk patients in intensive care. Clin. J. Am. Soc. Nephrol. 10, 187–196 (2015).
Google Scholar
Soranno, D. E. et al. The role of sex and gender in acute kidney injury-consensus statements from the 33rd Acute Disease Quality Initiative. Kidney Int. 107, 606–616 (2025).
Google Scholar
Neugarten, J., Golestaneh, L. & Kolhe, N. V. Sex differences in acute kidney injury requiring dialysis. BMC Nephrol. 19, 131 (2018).
Google Scholar
Wichmann, M. W., Inthorn, D., Andress, H. J. & Schildberg, F. W. Incidence and mortality of severe sepsis in surgical intensive care patients: the influence of patient gender on disease process and outcome. Intensive Care Med. 26, 167–172 (2000).
Google Scholar
Curtis, L. M. Sex and gender differences in AKI. Kidney360 5, 160–167 (2024).
Google Scholar
Neugarten, J., Sandilya, S., Singh, B. & Golestaneh, L. Sex and the risk of AKI following cardio-thoracic surgery: a meta-analysis. Clin. J. Am. Soc. Nephrol. 11, 2113–2122 (2016).
Google Scholar
Cheng, Y. et al. Incidence, risk factors and outcome of postoperative acute kidney injury in China. Nephrol. Dial. Transpl. 39, 967–977 (2024).
Google Scholar
Goldstein, S. L. et al. Consensus-based recommendations on priority activities to address acute kidney injury in children: a modified Delphi consensus statement. JAMA Netw. Open 5, e2229442 (2022).
Google Scholar
Mottes, T. et al. Pediatric AKI in the real world: changing outcomes through education and advocacy — a report from the 26th Acute Disease Quality Initiative (ADQI) consensus conference. Pediat. Nephrol. 39, 1005–1014 (2024).
Google Scholar
Lameire, N., Van Biesen, W. & Vanholder, R. Epidemiology of acute kidney injury in children worldwide, including developing countries. Pediatr. Nephrol. 32, 1301–1314 (2017).
Google Scholar
Kaddourah, A. et al. Epidemiology of acute kidney injury in critically ill children and young adults. N. Eng. J. Med. 376, 11–20 (2017).
Google Scholar
Sutherland, S. M. et al. AKI in hospitalized children: epidemiology and clinical associations in a national cohort. Clin. J. Am. Soc. Nephrol. 8, 1661–1669 (2013).
Google Scholar
Rutledge, A. D. et al. Incidence, risk factors, and outcomes associated with recurrent neonatal acute kidney injury in the AWAKEN study. JAMA Netw. Open 7, e2355307 (2024).
Google Scholar
Selewski, D. T. et al. Quality improvement goals for pediatric acute kidney injury: pediatric applications of the 22nd Acute Disease Quality Initiative (ADQI) conference. Pediatr. Nephrol. 36, 733–746 (2021).
Google Scholar
Sarker, R. et al. The WHO has declared the end of pandemic phase of COVID-19: way to come back in the normal life. Health Sci. Rep. 6, e1544 (2023).
Google Scholar
Kolhe, N. V., Fluck, R. J., Selby, N. M. & Taal, M. W. Acute kidney injury associated with COVID-19: a retrospective cohort study. PLoS Med. 17, e1003406 (2020).
Google Scholar
Checcucci, E. et al. Health Information Technology Usability Evaluation Scale (Health-ITUES) and user-experience questionnaire (UEQ) for 3D Intraoperative Cognitive Navigation (ICON3DTM) system for urological procedures. Medicina 59, 624 (2023).
Google Scholar
Hsiao, C. Y. et al. Acute kidney injury in patients with COVID-19 compared to those with influenza: a systematic review and meta-analysis. Front. Med. 10, 1252990 (2023).
Google Scholar
Nugent, J. et al. Assessment of acute kidney injury and longitudinal kidney function after hospital discharge among patients with and without COVID-19. JAMA Netw. Open 4, e211095 (2021).
Google Scholar
Cerda, J. et al. Promoting kidney function recovery in patients with AKI requiring RRT. Clin. J. Am. Soc. Nephrol. 10, 1859–1867 (2015).
Google Scholar
Lumlertgul, N. et al. Changing epidemiology of acute kidney injury in critically ill patients with COVID-19: a prospective cohort. Ann. Intensive Care 12, 118 (2022).
Google Scholar
Lumlertgul, N. et al. Acute kidney injury prevalence, progression and long-term outcomes in critically ill patients with COVID-19: a cohort study. Ann. Intensive Care 11, 123 (2021).
Google Scholar
Sullivan, M. K. et al. Acute kidney injury in patients hospitalized with COVID-19 from the ISARIC WHO CCP-UK study: a prospective, multicentre cohort study. Nephrol. Dial. Transpl. 37, 271–284 (2022).
Google Scholar
Wainstein, M. et al. Association of country income level with the characteristics and outcomes of critically ill patients hospitalized with acute kidney injury and COVID-19. Kidney Int. Rep. 8, 1514–1530 (2023).
Google Scholar
Charytan, D. M. et al. Decreasing incidence of acute kidney injury in patients with COVID-19 critical illness in New York City. Kidney Int. Rep. 6, 916–927 (2021).
Google Scholar
Selby, N. M. et al. An organizational-level program of intervention for AKI: a pragmatic stepped wedge cluster randomized trial. J. Am. Soc. Nephrol. 30, 505–515 (2019).
Google Scholar
Rhee, H. et al. Influence of baseline kidney function on patient and kidney outcomes in patients with COVID-19: a multi-national observational study. J. Clin. Med. 14, 1212 (2025).
Google Scholar
Bagshaw, S. M., George, C., Bellomo, R. & Committee, A. D. M. Changes in the incidence and outcome for early acute kidney injury in a cohort of Australian intensive care units. Crit. Care 11, R68 (2007).
Google Scholar
Bagshaw, S. M., George, C., Bellomo, R. & Committee, A. D. M. Early acute kidney injury and sepsis: a multicentre evaluation. Crit. Care 12, R47 (2008).
Google Scholar
Peerapornratana, S., Manrique-Caballero, C. L., Gomez, H. & Kellum, J. A. Acute kidney injury from sepsis: current concepts, epidemiology, pathophysiology, prevention and treatment. Kidney Int. 96, 1083–1099 (2019).
Google Scholar
Ikizler, T. A. et al. A prospective cohort study of acute kidney injury and kidney outcomes, cardiovascular events, and death. Kidney Int. 99, 456–465 (2021).
Google Scholar
Uchino, S. et al. Acute renal failure in critically ill patients: a multinational, multicenter study. JAMA 294, 813–818 (2005).
Google Scholar
Rudd, K. E. et al. The global burden of sepsis: barriers and potential solutions. Crit. Care 22, 232 (2018).
Google Scholar
Liu, J. et al. Rates, predictors, and mortality of sepsis-associated acute kidney injury: a systematic review and meta-analysis. BMC Nephrol. 21, 318 (2020).
Google Scholar
Yoshimoto, K., Komaru, Y., Iwagami, M. & Doi, K. Acute kidney injury in sepsis: evidence from Asia. Semin. Nephrol. 40, 489–497 (2020).
Google Scholar
Yoon, S. Y., Kim, J. S., Jeong, K. H. & Kim, S. K. Acute kidney injury: biomarker-guided diagnosis and management. Medicina 58, 340 (2022).
Google Scholar
Lyrio, R. et al. Chemotherapy-induced acute kidney injury: epidemiology, pathophysiology, and therapeutic approaches. Front. Nephrol. 4, 1436896 (2024).
Google Scholar
Christiansen, C. F., Johansen, M. B., Langeberg, W. J., Fryzek, J. P. & Sørensen, H. T. Incidence of acute kidney injury in cancer patients: a Danish population-based cohort study. Eur. J. Intern. Med. 22, 399–406 (2011).
Google Scholar
Kitchlu, A. et al. Acute kidney injury in patients receiving systemic treatment for cancer: a population-based cohort study. J. Natl Cancer Inst. 111, 727–736 (2019).
Google Scholar
Cheng, Y. et al. Epidemiology and outcomes of acute kidney injury in hospitalized cancer patients in China. Int. J. Cancer 144, 2644–2650 (2019).
Google Scholar
Calças Marques, R. et al. Severe acute kidney injury in hospitalized cancer patients: epidemiology and predictive model of renal replacement therapy and in-hospital mortality. Cancers 16, 561 (2024).
Google Scholar
Rosner, M. H., Darmon, M. & Ostermann, M. Onco-nephrology: what the intensivist needs to know. Intensive Care Med. 48, 1234–1236 (2022).
Google Scholar
Sousa, C. et al. Post-renal acute kidney injury in patients with cancer: clinical presentation and kidney and patient outcomes. J. Onco-Nephrol. 7, 120–129 (2023).
Google Scholar
Perazella, M. A. & Rosner, M. H. Drug-induced acute kidney injury. Clin. J. Am. Soc. Nephrol. 17, 1220–1233 (2022).
Google Scholar
Yarandi, N. & Shirali, A. C. Onconephrology: core curriculum 2023. Am. J. Kidney Dis. 82, 743–761 (2023).
Google Scholar
Meraz-Munoz, A., Langote, A. K. D. J., Izzedine, H. & Gudsoorkar, P. Acute kidney injury in the patient with cancer. Diagnostics 11, 611 (2021).
Google Scholar
Hanna, P. E. et al. Adverse kidney outcomes of CDK 4/6 inhibitors for metastatic breast cancer. npj Breast Cancer 9, 70 (2023).
Google Scholar
Braet, P., Sartò, G. V. R., Pirovano, M., Sprangers, B. & Cosmai, L. Treatment of acute kidney injury in cancer patients. Clin. Kidney J. 15, 873–884 (2022).
Google Scholar
Herrmann, S. M. & Perazella, M. A. Immune checkpoint inhibitors and immune-related adverse renal events. Kidney Int. Rep. 5, 1139–1148 (2020).
Google Scholar
Izzedine, H. & Perazella, M. A. Anticancer drug-induced acute kidney injury. Kidney Int. Rep. 2, 504–514 (2017).
Google Scholar
Yoon, S. Y. et al. Global burden of anticancer drug-induced acute kidney injury and tubulointerstitial nephritis from 1967 to 2023. Sci. Rep. 14, 16124 (2024).
Google Scholar
Gupta, S. et al. AKI treated with renal replacement therapy in critically Ill patients with COVID-19. J. Am. Soc. Nephrol. 32, 161–176 (2021).
Google Scholar
Piscitani, L., Sirolli, V., Di Liberato, L., Morroni, M. & Bonomini, M. Nephrotoxicity associated with novel anticancer agents (aflibercept, dasatinib, nivolumab): case series and nephrological considerations. Int. J. Mol. Sci. 21, 4878 (2020).
Google Scholar
Duley, L. The global impact of pre-eclampsia and eclampsia. Semin. Perinatol. 33, 130–137 (2009).
Google Scholar
Arrayhani, M., El Youbi, R. & Sqalli, T. Pregnancy-related acute kidney injury: experience of the nephrology unit at the university hospital of Fez, Morocco. Int. Sch. Res. Not. 2013, 109034 (2013).
Cooke, W. R. et al. Incidence, aetiology and outcomes of obstetric-related acute kidney injury in Malawi: a prospective observational study. BMC Nephrol. 19, 25 (2018).
Google Scholar
Gaber, T. Z. et al. Acute kidney injury during pregnancy and puerperium: an Egyptian hospital-based study. J. Nephrol. 34, 1611–1619 (2021).
Google Scholar
Gurrieri, C. et al. Kidney injury during pregnancy: associated comorbid conditions and outcomes. Arch. Gynecol. Obst. 286, 567–573 (2012).
Google Scholar
Huang, C. & Chen, S. Acute kidney injury during pregnancy and puerperium: a retrospective study in a single center. BMC Nephrol. 18, 146 (2017).
Google Scholar
Meca, D.-C., Varlas, V. N., Mehedințu, C. & Cîrstoiu, M. M. Correlations between maternal and fetal outcomes in pregnant women with kidney failure. J. Clin. Med. 12, 832 (2023).
Google Scholar
Sachan, R., Shukla, S., Shyam, R., Sachan, P. L. & Patel, M. L. Feto-maternal outcome of pregnancy related acute kidney injury in a North Indian population. J. Fam. Community Med. 29, 204 (2022).
Google Scholar
Thakur, G. et al. Acute kidney injury and its outcome following maternal near-miss event: a prospective observational study from a tertiary care hospital. Obstet. Med. 16, 48–51 (2023).
Google Scholar
Coles, H., Steer, P., Hughes, P. & Cauldwell, M. Factors associated with acute kidney injury during delivery or the postpartum period: a case control study. Eur. J. Obst. Gynecol. Reprod. Biol. 261, 200–204 (2021).
Google Scholar
Gama, R. M. et al. Acute kidney injury e-alerts in pregnancy: rates, recognition and recovery. Nephrol. Dial. Transplant. 36, 1023–1030 (2021).
Google Scholar
Gayathiri, M., Suganya, S. & & Arul A study of AKI in pregnancy and puerperium. Indian J. Obstet. Gynecol. Res. 7, 344–347 (2020).
Google Scholar
Prakash, J. et al. Acute kidney injury in pregnancy with special reference to pregnancy-specific disorders: a hospital based study (2014–2016). J. Nephrol. 31, 79–85 (2018).
Google Scholar
Rage, H. I., Jha, P. K., Hashi, H. A. & Abdillahi, N. I. Pregnancy-related AKI: a tertiary care hospital experience in Somaliland. Kidney Int. Rep. 8, 388–391 (2023).
Google Scholar
Bentata, Y. et al. Acute kidney injury according to KDIGO stages and maternal mortality in the intensive care unit. Intensive Care Med. 41, 555–556 (2015).
Google Scholar
Mehrabadi, A. et al. Hypertensive disorders of pregnancy and the recent increase in obstetric acute renal failure in Canada: population based retrospective cohort study. BMJ 349, g4731 (2014).
Google Scholar
Mehrabadi, A., Dahhou, M., Joseph, K. S. & Kramer, M. S. Investigation of a rise in obstetric acute renal failure in the United States, 1999–2011. Obst. Gynecol. 127, 899–906 (2016).
Google Scholar
Abderraman, G. M., Charfadine, S. & Hissein, A. Outcome of acute kidney injury in pregnancy in N’Djamena, Chad. Open J. Nephrol. 13, 369–377 (2023).
Google Scholar
Kharkongor, D. et al. Acute kidney injury in obstetrics: hospital-based cohort study. Trop. Doct. 53, 356–361 (2023).
Google Scholar
Ruggajo, P. J. et al. Prevalence, risk factors and short-term outcomes of acute kidney injury in women with obstetric complications in Dar es Salaam, Tanzania. Tanz. Med. J. 33, 14–29 (2022).
Fakhouri, F. & Deltombe, C. Pregnancy-related acute kidney injury in high income countries: still a critical issue. J. Nephrol. 30, 767–771 (2017).
Google Scholar
Escobar, M. F. et al. Synthesis of evidence for managing hypertensive disorders of pregnancy in low middle-income countries: a scoping review. BMC Pregnancy Childbirth 24, 622 (2024).
Google Scholar
Anvar, M. I., Talwar, S., Mallapur, S. & ANVAR, M. I. A retrospective study on clinical outcomes of pregnancy-related acute kidney injury patients at a South Indian tertiary care hospital. Cureus 15, e49610 (2023).
Beers, K. et al. Racial and ethnic disparities in pregnancy-related acute kidney injury. Kidney360 1, 169 (2020).
Google Scholar
Nadim, M. K. & Garcia-Tsao, G. Acute kidney injury in patients with cirrhosis. N. Engl. J. Med. 388, 733–745 (2023).
Google Scholar
Desai, A. P. et al. Changing epidemiology and outcomes of acute kidney injury in hospitalized patients with cirrhosis — a US population-based study. J. Hepatol. 73, 1092–1099 (2020).
Google Scholar
Patidar, K. R. et al. Incidence and outcomes of acute kidney injury including hepatorenal syndrome in hospitalized patients with cirrhosis in the US. J. Hepatol. 79, 1408–1417 (2023).
Google Scholar
Nadim, M. K. et al. Hepatorenal syndrome: the 8th International Consensus Conference of the Acute Dialysis Quality Initiative (ADQI) group. Crit. Care 16, R23 (2012).
Google Scholar
Angeli, P. et al. Diagnosis and management of acute kidney injury in patients with cirrhosis: revised consensus recommendations of the International Club of Ascites. J. Hepatol. 62, 968–974 (2015).
Google Scholar
Nadim, M. K. et al. Acute kidney injury in patients with cirrhosis: Acute Disease Quality Initiative (ADQI) and International Club of Ascites (ICA) joint multidisciplinary consensus meeting. J. Hepatol. 81, 163–183 (2024).
Google Scholar
Nadim, M. K. et al. Cardiac and vascular surgery-associated acute kidney injury: the 20th International Consensus Conference of the ADQI (Acute Disease Quality Initiative) group. J. Am. Heart Assoc. 7, e008834 (2018).
Google Scholar
Ostermann, M., Cennamo, A., Meersch, M. & Kunst, G. A narrative review of the impact of surgery and anaesthesia on acute kidney injury. Anaesthesia 75, e121–e133 (2020).
Google Scholar
Hu, J. et al. Global incidence and outcomes of adult patients with acute kidney injury after cardiac surgery: a systematic review and meta-analysis. J. Cardiothorac. Vasc. Anesth. 30, 82–89 (2016).
Google Scholar
Ostermann, M. & Cerdá, J. The burden of acute kidney injury and related financial issues. Contrib. Nephrol. 193, 100–112 (2018).
Google Scholar
Edmiston, T. et al. What is the need for and access to trauma surgery in low- and middle-income countries? A scoping review. World J. Surg. 49, 1928–1940 (2025).
Google Scholar
Haines, R. W., Fowler, A. J., Kirwan, C. J. & Prowle, J. R. The incidence and associations of acute kidney injury in trauma patients admitted to critical care: a systematic review and meta-analysis. J. Trauma Acute Care Surg. 86, 141–147 (2019).
Google Scholar
Perkins, Z. B., Haines, R. W. & Prowle, J. R. Trauma-associated acute kidney injury. Curr. Opin. Crit. Care 25, 565–572 (2019).
Google Scholar
Long, B., Liang, S. Y. & Gottlieb, M. Crush injury and syndrome: a review for emergency clinicians. Am. J. Emerg. Med. 69, 180–187 (2023).
Google Scholar
Barsoum, R. S. Tropical acute renal failure. Contrib. Nephrol. 144, 44–52 (2004).
Google Scholar
Daher, F. et al. Acute kidney injury in a tropical country: a cohort study of 253 patients in an infectious diseases intensive care unit. Rev. Soc. Bras. Med. Trop. 47, 86–89 (2014).
Google Scholar
Jha, V. & Chugh, K. S. Community-acquired acute kidney injury in Asia. Semin. Nephrol. 28, 330–347 (2008).
Google Scholar
Pappas, G., Papadimitriou, P., Siozopoulou, V., Christou, L. & Akritidis, N. The globalization of leptospirosis: worldwide incidence trends. Int. J. Infect. Dis. 12, 351–357 (2008).
Google Scholar
Severe falciparum malaria. World Health Organization, Communicable Diseases Cluster. Trans. R. Soc. Trop. Med. Hyg. 94, S1–S90 (2000).
Kusirisin, P., da Silva Junior, G. B., Sitprija, V. & Srisawat, N. Acute kidney injury in the tropics. Nephrology 28, 5–20 (2023).
Google Scholar
Kute, V. B. et al. Plasmodium vivax malaria-associated acute kidney injury, India, 2010–2011. Emerg. Infect. Dis. 18, 842–845 (2012).
Google Scholar
Silva, G. B. D. J., Pinto, J. R., Barros, E. J. G., Farias, G. M. N. & Daher, E. F. Kidney involvement in malaria: an update. Rev. Inst. Med. Trop. Sao Paulo 59, e53 (2017).
Google Scholar
Sitprija, V., Indraprasit, S., Pochanugool, C., Benyajati, C. & Piyaratn, P. Renal failure in malaria. Lancet 1, 185–188 (1967).
Google Scholar
Sitprija, V., Vongsthongsri, M., Poshyachinda, V. & Arthachinta, S. Renal failure in malaria: a pathophysiologic study. Nephron 18, 277–287 (1977).
Google Scholar
Silva Júnior, G. B. et al. RIFLE and acute kidney injury network classifications predict mortality in leptospirosis-associated acute kidney injury. Nephrology 16, 269–276 (2011).
Google Scholar
Sitprija, V. Renal involvement in human leptospirosis. Br. Med. J. 2, 656–658 (1968).
Google Scholar
Daher Ede, F., de Abreu, K. L. & da Silva Junior, G. B. Leptospirosis-associated acute kidney injury. J. Bras. Nefrol. 32, 400–407 (2010).
Google Scholar
Batte, A., Shahrin, L., Claure-Del Granado, R., Luyckx, V. A. & Conroy, A. L. Infections and acute kidney injury: a global perspective. Semin. Nephrol. 43, 151466 (2023).
Google Scholar
Mallhi, T. H. et al. Dengue-induced acute kidney injury (DAKI): a neglected and fatal complication of dengue viral infection — a systematic review. JCPSP 25, 828–834 (2015).
Google Scholar
Awad, A. A. et al. Predictors of acute kidney injury in dengue patients: a systematic review and meta-analysis. Virol. J. 21, 223 (2024).
Google Scholar
Kanjanabuch, T. & Sitprija, V. Snakebite nephrotoxicity in Asia. Semin. Nephrol. 28, 363–372 (2008).
Google Scholar
Pinho, F. M. O., Yu, L. & Burdmann, E. A. Snakebite-induced acute kidney injury in Latin America. Semin. Nephrol. 28, 354–362 (2008).
Google Scholar
Xie, C. et al. Clinical features of severe wasp sting patients with dominantly toxic reaction: analysis of 1091 cases. PLoS ONE 8, e83164 (2013).
Google Scholar
Reimann, H. A. & Sukaton, R. U. Djenkol bean poisoning (djenkolism); a cause of hematuria and anuria. Am. J. Med. Sci. 232, 172–174 (1956).
Google Scholar
Bye, S. N., Coetzer, T. H. & Dutton, M. F. An enzyme immunoassay for atractyloside, the nephrotoxin of Callilepis laureola (Impila). Toxicon 28, 997–1000 (1990).
Google Scholar
Seedat, Y. K. & Hitchcock, P. J. Acute renal failure from Callilepsis laureola. S Afr. Med. J. 45, 832–833 (1971).
Google Scholar
Lee, K. G. Star fruit intoxication with acute kidney injury. Clin. Med. 12, 494 (2012).
Google Scholar
McClain, J. L., Hause, D. W. & Clark, M. A. Amanita phalloides mushroom poisoning: a cluster of four fatalities. J. Forens. Sci. 34, 83–87 (1989).
Google Scholar
Gao, H., Yang, Z. S. & Jin, S. X. Primary observations on distal renal tubule acidosis in 177 cases caused by gossypol intoxication. Zhonghua Nei Ke Za Zhi 24, 419–421 (1985).
Google Scholar
Yang, B. et al. Nephrotoxicity and Chinese herbal medicine. Clin. J. Am. Soc. Nephrol. 13, 1605–1611 (2018).
Google Scholar
Macedo, E., Garcia-Garcia, G., Mehta, R. L. & Rocco, M. V. International Society of Nephrology 0 by 25 project: lessons learned. Ann. Nutr. Metab. 74, 45–50 (2019).
Google Scholar
Loutradis, C. et al. Acute kidney injury is more common in men than women after accounting for socioeconomic status, ethnicity, alcohol intake and smoking history. Biol. Sex Differ. 12, 30 (2021).
Google Scholar
Hounkpatin, H. O. et al. The association of socioeconomic status with incidence and outcomes of acute kidney injury. Clin. Kidney J. 13, 245–252 (2020).
Google Scholar
Perico, N., Askenazi, D., Cortinovis, M. & Remuzzi, G. Maternal and environmental risk factors for neonatal AKI and its long-term consequences. Nat. Rev. Nephrol. 14, 688–703 (2018).
Google Scholar
Jensen, S. K. et al. Regional variation in incidence and prognosis of acute kidney injury. Nephrol. Dial. Transpl. 39, 1171–1180 (2024).
Google Scholar
Vanholder, R. et al. Inequities in kidney health and kidney care. Nat. Rev. Nephrol. 19, 694–708 (2023).
Google Scholar
Kashani, K. et al. Acute kidney injury risk assessment: differences and similarities between resource-limited and resource-rich countries. Kidney Int. Rep. 2, 519–529 (2017).
Google Scholar
Awdishu, L. et al. Rationale and design of the genetic contribution to drug induced renal injury (DIRECT) study. Kidney Int. Rep. 1, 288–298 (2016).
Google Scholar
Meena, J., Thomas, C. C., Kumar, J., Mathew, G. & Bagga, A. Biomarkers for prediction of acute kidney injury in pediatric patients: a systematic review and meta-analysis of diagnostic test accuracy studies. Pediat. Nephrol. 38, 3241–3251 (2023).
Google Scholar
Claure-Del Granado, R., Macedo, E. & Chávez-Íñiguez, J. S. Biomarkers for early diagnosis of AKI: could it backfire? Kidney360 3, 1780–1784 (2022).
Google Scholar
Legrand, M. et al. Sepsis-associated acute kidney injury: recent advances in enrichment strategies, sub-phenotyping and clinical trials. Crit. Care 28, 92 (2024).
Google Scholar
Barracca, A. et al. Digital health: a new frontier. J. Transl. Crit. Care Med. 5, e00018 (2023).
Google Scholar
Bharadwaj, M., Bengtson, M., Golverdingen, M., Waling, L. & Dekker, C. Diagnosing point-of-care diagnostics for neglected tropical diseases. PLoS Negl. Trop. Dis. 15, e0009405 (2021).
Google Scholar
Costa, A. D. T. & Santos, J. F. L. Editorial: New strategies and technologies enabling point of care diagnosis of neglected or tropical diseases. Front. Cell Infect. Microbiol. 12, 1089088 (2022).
Google Scholar
Kaminstein, D. Point-of-care ultrasound for tropical disease: implications for clinical decision-making. Am. J. Trop. Med. Hyg. 103, 542–543 (2020).
Google Scholar
Raimann, J. G., Riella, M. C. & Levin, N. W. International Society of Nephrology’s 0by25 initiative (zero preventable deaths from acute kidney injury by 2025): focus on diagnosis of acute kidney injury in low-income countries. Clin. Kidney J. 11, 12–19 (2018).
Google Scholar
Calice-Silva, V. et al. Diagnostic performance of salivary urea nitrogen dipstick to detect and monitor acute kidney disease in patients with malaria. Malaria J. 17, 477 (2018).
Google Scholar
Evans, R. D. R. et al. A salivary urea nitrogen dipstick to detect obstetric-related acute kidney disease in Malawi. Kidney Int. Rep. 3, 178–184 (2018).
Google Scholar
Rizo-Topete, L. M., Rosner, M. H. & Ronco, C. Acute kidney injury risk assessment and the nephrology rapid response team. Blood Purif. 43, 82–88 (2017).
Google Scholar
Kane-Gill, S. L., Meersch, M. & Bell, M. Biomarker-guided management of acute kidney injury. Curr. Opin. Crit. Care 26, 556–562 (2020).
Google Scholar
Cerda, J. et al. Acute kidney injury recognition in low- and middle-income countries. Kidney Int. Rep. 2, 530–543 (2017).
Google Scholar
Macedo, E. et al. Quality of care after AKI development in the hospital: consensus from the 22nd Acute Disease Quality Initiative (ADQI) conference. Eur. J. Intern. Med. 80, 45–53 (2020).
Google Scholar
Kashani, K. et al. Quality improvement goals for acute kidney injury. Clin. J. Am. Soc. Nephrol. 14, 941–953 (2019).
Google Scholar
Claure-Del Granado, R., Casas-Aparicio, G., Rosa-Diez, G., Rizo-Topete, L. & Ponce, D. Renal replacement therapy for acute kidney injury in COVID-19 patients in Latin America. Kidney Blood Press. Res. 45, 775–783 (2020).
Google Scholar
Ferraz, F., Rodrigues, C. I. S., Gatto, G. C. & Sá, N. M. Differences and inequalities in relation to access to renal replacement therapy in the BRICS countries. Cien Saude Colet. 22, 2175–2185 (2017).
Google Scholar
Liyanage, T. et al. Worldwide access to treatment for end-stage kidney disease: a systematic review. Lancet 385, 1975–1982 (2015).
Google Scholar
Ostermann, M., Bagshaw, S. M., Lumlertgul, N. & Wald, R. Indications for and timing of initiation of KRT. Clin. J. Am. Soc. Nephrol. 18, 113–120 (2023).
Google Scholar
Forni, L. G. et al. Renal recovery after acute kidney injury. Intensive Care Med. 43, 855–866 (2017).
Google Scholar
Chawla, L. S. et al. Acute kidney disease and renal recovery: consensus report of the Acute Disease Quality Initiative (ADQI) 16 workgroup. Nat. Rev. Nephrol. 13, 241–257 (2017).
Google Scholar
Kellum, J. A., Sileanu, F. E., Bihorac, A., Hoste, E. A. & Chawla, L. S. Recovery after acute kidney injury. Am. J. Resp. Crit. Care Med. 195, 784–791 (2017).
Google Scholar
Siew, E. D. et al. Timing of recovery from moderate to severe AKI and the risk for future loss of kidney function. Am. J. Kidney Dis. 75, 204–213 (2020).
Google Scholar
See, E. J. et al. Long-term risk of adverse outcomes after acute kidney injury: a systematic review and meta-analysis of cohort studies using consensus definitions of exposure. Kidney Int. 95, 160–172 (2019).
Google Scholar
Haines, R. W., Powell-Tuck, J., Leonard, H., Crichton, S. & Ostermann, M. Long-term kidney function of patients discharged from hospital after an intensive care admission: observational cohort study. Sci. Rep. 11, 9928 (2021).
Google Scholar
Chaïbi, K. et al. Long-term outcomes after severe acute kidney injury in critically ill patients: the SALTO study. Ann. Intensive Care 13, 18 (2023).
Google Scholar
McNicholas, B., Akcan Arikan, A. & Ostermann, M. Quality of life after acute kidney injury. Curr. Opin. Crit. Care 29, 566–579 (2023).
Google Scholar
Muiru, A. N. et al. Risk for chronic kidney disease progression after acute kidney injury: findings from the chronic renal insufficiency cohort study. Ann. Intern. Med. 176, 961–968 (2023).
Google Scholar
Gomez, H. et al. Persistent severe acute kidney injury is a major modifiable determinant of outcome during critical illness. Intensive Care Med. 51, 542–555 (2025).
Google Scholar
Endre, Z., Rebora, P. & Ostermann, M. Persistent severe AKI is bad — where to go now? Intensive Care Med. 51, 954–956 (2025).
Google Scholar
Koyner, J. L. et al. Health care resource utilization and costs of persistent severe acute kidney injury (PS-AKI) among hospitalized stage 2/3 AKI patients. Kidney360 4, 316–325 (2023).
Google Scholar
Vanmassenhove, J., Vanholder, R. & Lameire, N. Points of concern in post acute kidney injury management. Nephron 138, 92–103 (2018).
Google Scholar
Silver, S. A. et al. Association of an acute kidney injury follow-up clinic with patient outcomes and care processes: a cohort study. Am. J. Kidney Dis. 81, 554–563.e551 (2023).
Google Scholar
Thanapongsatorn, P. et al. Comprehensive versus standard care in post-severe acute kidney injury survivors, a randomized controlled trial. Crit. Care 25, 322 (2021).
Google Scholar
Brar, S., Ye, F., James, M. T., Harrison, T. G. & Pannu, N. Processes of care after hospital discharge for survivors of acute kidney injury: a population-based cohort study. Am. J. Kidney Dis. 83, 216–228 (2024).
Google Scholar
Silver, S. A. et al. What insights do patients and caregivers have on acute kidney injury and posthospitalisation care? A single-centre qualitative study from Toronto, Canada. BMJ Open. 8, e021418 (2018).
Google Scholar
US National Library of Medicine. ClinicalTrials.gov (2025).
Morton, R. L. et al. Impact of educational attainment on health outcomes in moderate to severe CKD. Am. J. Kidney Dis. 67, 31–39 (2016).
Google Scholar
Jamison, D. T. et al. (eds.) Disease Control Priorities: Improving Health and Reducing Poverty (The World Bank, 2017).
Boulware, L. E. & Mohottige, D. The seen and the unseen: race and social inequities affecting kidney care. Clin. J. Am. Soc. Nephrol. 16, 815–817 (2021).
Google Scholar
Rizzolo, K. & Cervantes, L. Immigration status and end-stage kidney disease: role of policy and access to care. Semin. Dial. 33, 513–522 (2020).
Google Scholar
Hall, Y. N., O’Hare, A. M., Young, B. A., Boyko, E. J. & Chertow, G. M. Neighborhood poverty and kidney transplantation among US Asians and Pacific Islanders with end-stage renal disease. Am. J. Transpl. 8, 2402–2409 (2008).
Google Scholar
Sawhney, S. et al. Care processes and outcomes of deprivation across the clinical course of kidney disease: findings from a high-income country with universal healthcare. Nephrol. Dial. Transpl. 38, 1170–1182 (2023).
Google Scholar
Htay, H. et al. Global access of patients with kidney disease to health technologies and medications: findings from the Global Kidney Health Atlas project. Kidney Int. Suppl. 8, 64–73 (2018).
Google Scholar
Anandh, U., Meena, P., Karam, S. & Luyckx, V. Social, political and legal determinants of kidney health: perspectives from lower- and middle-income countries with a focus on India. Front. Nephrol. 2, 1024667 (2022).
Google Scholar
Rewa, O. & Bagshaw, S. M. Acute kidney injury — epidemiology, outcomes and economics. Nat. Rev. Nephrol. 10, 193–207 (2014).
Google Scholar
Li, P. K., Burdmann, E. A. & Mehta, R. L. Acute kidney injury: global health alert. Kidney Int. 83, 372–376 (2013).
Google Scholar
Akcan Arikan, A., Ostermann, M., Goldstein, S. L. & Kellum, J. A. Sepsis criteria and kidney function: eliminating sex, age and economic status biases. Nat. Rev. Nephrol. 21, 565–575 (2025).
Google Scholar
Gansevoort, R. T. et al. What should European nephrology do with the new CKD-EPI equation? Nephrol. Dial. Transpl. 38, 1–6 (2023).
Google Scholar
Nankivell, B. J., Nankivell, L. F. J., Elder, G. J. & Gruenewald, S. M. How unmeasured muscle mass affects estimated GFR and diagnostic inaccuracy. eClinicalMedicine 29-30, 100662 (2020).
Google Scholar
Rachel, M., Galiniak, S., Biesiadecki, M. & Gala-Bladzinska, A. Renal function in patients with cystic fibrosis: a single-center study. Int. J. Env. Res. Public. Health 19, 5454 (2022).
Google Scholar
Scanlon, L. A., O’Hara, C., Garbett, A., Barker-Hewitt, M. & Barriuso, J. Developing an agnostic risk prediction model for early AKI detection in cancer patients. Cancers 13, 4182 (2021).
Google Scholar
Choon, X. Y. et al. Discharge documentation and follow-up of critically ill patients with acute kidney injury treated with kidney replacement therapy: a retrospective cohort study. Front. Med. 8, 710228 (2021).
Google Scholar
Switzer, G. E. et al. Patient-reported experiences after acute kidney injury across multiple health-related quality-of-life domains. Kidney360 3, 426–434 (2022).
Google Scholar
Bonfield, B. Impact of providing patient information leaflets prior to hospital discharge to patients with acute kidney injury: a quality improvement project. BMJ Open Qual. 10, e001359 (2021).
Google Scholar
Natale, P. et al. Perspectives and experiences of patients with AKI: a systematic review. Clin. J. Am. Soc. Nephrol. 20, 326–336 (2025).
Google Scholar
Diamantidis, C. J. et al. What do acute kidney injury survivors want to know about their condition: a qualitative study. Kidney Med. 4, 100423 (2022).
Google Scholar
Akcan-Arikan, A. Pediatric acute kidney injury — deadly now, costly later, and a public health burden. Pediat. Crit. Care Med. 16, 774–775 (2015).
Google Scholar
Dasta, J. F., Kane-Gill, S. L., Durtschi, A. J., Pathak, D. S. & Kellum, J. A. Costs and outcomes of acute kidney injury (AKI) following cardiac surgery. Nephrol. Dial. Transpl. 23, 1970–1974 (2008).
Google Scholar
Filiberto, A. C. et al. Persistent acute kidney injury is associated with poor outcomes and increased hospital cost in vascular surgery. Ann. Vasc. Surg. 98, 342–349 (2024).
Google Scholar
Kashani, K. B. et al. Digital health and acute kidney injury: consensus report of the 27th Acute Disease Quality Initiative workgroup. Nat. Rev. Nephrol. 19, 807–818 (2023).
Google Scholar
Lahoti, A., Nates, J. L., Wakefield, C. D., Price, K. J. & Salahudeen, A. K. Costs and outcomes of acute kidney injury in critically ill patients with cancer. J. Support. Oncol. 9, 149–155 (2011).
Google Scholar
Raina, R., Sethi, S., Aitharaju, V., Vadhera, A. & Haq, I. Epidemiology data on the cost and outcomes associated with pediatric acute kidney injury. Pediat. Res. 94, 1385–1391 (2023).
Google Scholar
Jha, V. et al. Global economic burden associated with chronic kidney disease: a pragmatic review of medical costs for the inside CKD research programme. Adv. Ther. 40, 4405–4420 (2023).
Google Scholar
Monard, C. et al. Economic burden of in-hospital AKI: a one-year analysis of the nationwide French hospital discharge database. BMC Nephrol. 24, 343 (2023).
Google Scholar
Wu, V. C. et al. Acute-on-chronic kidney injury at hospital discharge is associated with long-term dialysis and mortality. Kidney Int. 80, 1222–1230 (2011).
Google Scholar
Engelman, D. T. et al. Using urinary biomarkers to reduce acute kidney injury following cardiac surgery. J. Thorac. Cardiovasc. Surg. 160, 1235–1246 e1232 (2020).
Google Scholar
Chen, J. J. et al. Electronic alert systems for patients with acute kidney injury: a systematic review and meta-analysis. JAMA Netw. Open 7, e2430401 (2024).
Google Scholar
Kolhe, N. V., Muirhead, A. W., Wilkes, S. R., Fluck, R. J. & Taal, M. W. The epidemiology of hospitalised acute kidney injury not requiring dialysis in England from 1998 to 2013: retrospective analysis of hospital episode statistics. Int. J. Clin. Pract. 70, 330–339 (2016).
Google Scholar
Grams, M. E. et al. Explaining the racial difference in AKI incidence. J. Am. Soc. Nephrol. 25, 1834–1841 (2014).
Google Scholar
Sustainable Development Goals: the 17 goals. The United Nations (2015).
Feehally, J. The ISN 0by25 Global Snapshot Study. Ann. Nutr. Metab. 68, 29–31 (2016).
Google Scholar
Bello, A. K. et al. Global Kidney Health Atlas (GKHA): design and methods. Kidney Int. Suppl. 7, 145–153 (2017).
Google Scholar
Freidin, N., Hayes, E. & Struthers, S. A. Implications of climate change on acute kidney injury. Curr. Opin. Nephrol. Hypertens. 33, 83–88 (2024).
Google Scholar
Goldfarb, D. S. & Patel, A. A. Climate change and its implications for kidney health. Curr. Opin. Urol. 34, 377–383 (2024).
Google Scholar
Guo, C. et al. Impact of heat on emergency hospital admissions related to kidney diseases in Texas: uncovering racial disparities. Sci. Total. Environ. 909, 168377 (2024).
Google Scholar
Green, R. S. et al. The effect of temperature on hospital admissions in nine California counties. Int. J. Public Health 55, 113–121 (2010).
Google Scholar
Anderson, B. G. & Bell, M. L. Weather-related mortality: how heat, cold, and heat waves affect mortality in the United States. Epidemiology 20, 205–213 (2009).
Google Scholar
Ulasi, I. I., Burdmann, E. A., Ijoma, C. K., Chou, L. F. & Yang, C. W. Neglected and emerging infections of the kidney. Semin. Nephrol. 43, 151472 (2023).
Google Scholar
Cheungpasitporn, W., Thongprayoon, C., Ronco, C. & Kashani, K. B. Generative AI in critical care nephrology: applications and future prospects. Blood Purif. 53, 871–883 (2024).
Google Scholar
Aminpour, F., Sadoughi, F. & Ahamdi, M. Utilization of open source electronic health record around the world: a systematic review. J. Res. Med. Sci. 19, 57–64 (2014).
Google Scholar
About International Telecommunication Union (ITU). ITU (2023).
Peng, Z. et al. Pragmatic studies for acute kidney injury: consensus report of the acute disease quality initiative (ADQI) 19 workgroup. J. Crit. Care 44, 337–344 (2018).
Google Scholar
Fuhrman, D. Y., Bagshaw, S. M., Goldstein, S. L., Legrand, M. & Shaw, A. D. Major adverse kidney events as an endpoint in acute kidney injury trials: is it time for a RE-MAKE? Intensive Care Med. 50, 1723–1724 (2024).
Google Scholar
Meersch, M. et al. Prevention of cardiac surgery-associated AKI by implementing the KDIGO guidelines in high risk patients identified by biomarkers: the PrevAKI randomized controlled trial. Intensive Care Med. 43, 1551–1561 (2017).
Google Scholar
Zarbock, A. et al. Prevention of cardiac surgery-associated acute kidney injury by implementing the KDIGO Guidelines in high-risk patients identified by biomarkers: the PrevAKI-multicenter randomized controlled trial. Anesth. Analg. 133, 292–302 (2021).
Google Scholar
de Geus, H. R. et al. The cardiac surgery-associated neutrophil gelatinase-associated lipocalin (CSA-NGAL) score: a potential tool to monitor acute tubular damage. J. Thorac. Cardiovasc. Surg. 151, 1476–1481 (2016).
Google Scholar
Gerhardt, L. M. S. & McMahon, A. P. Multi-omic approaches to acute kidney injury and repair. Curr. Opin. Biomed. Eng. 20, 100344 (2021).
Google Scholar
Chan, L. et al. AKI in hospitalized patients with COVID-19. J. Am. Soc. Nephrol. 32, 151–160 (2021).
Google Scholar
Si, R. et al. A novel lipid microbubble targeting e-selectin for ultrasound molecular imaging of acute kidney injury in rats. Mol. Pharm. 22, 6163–6173 (2025).
Google Scholar
Li, Y., Chen, L., Feng, L. & Li, M. Contrast-enhanced ultrasonography for acute kidney injury: a systematic review and meta-analysis. Ultrasound Med. Biol. 49, 1930–1939 (2023).
Google Scholar
Schneider, A., Johnson, L., Goodwin, M., Schelleman, A. & Bellomo, R. Bench-to-bedside review: contrast enhanced ultrasonography-a promising technique to assess renal perfusion in the ICU. Crit. Care 15, 157 (2011).
Google Scholar
Zhang, Y., Xiang, K., Pan, J., Cheng, R. & Sun, S. K. Noninvasive diagnosis of kidney dysfunction using a small-molecule manganese-based magnetic resonance imaging probe. Anal. Chem. 96, 3318–3328 (2024).
Google Scholar
Huang, X. et al. Non-invasive diagnosis of acute kidney injury using Mn-doped carbon dots-based magnetic resonance imaging. Biomater. Sci. 11, 4289–4297 (2023).
Google Scholar
Selby, N. M. & Duranteau, J. New imaging techniques in AKI. Curr. Opin. Crit. Care 26, 543–548 (2020).
Google Scholar
Caroli, A., Remuzzi, A. & Lerman, L. O. Basic principles and new advances in kidney imaging. Kidney Int. 100, 1001–1011 (2021).
Google Scholar
Quaglia, M. et al. Stem cell-derived extracellular vesicles as potential therapeutic approach for acute kidney injury. Front. Immunol. 13, 849891 (2022).
Google Scholar
Lao, X. Q., Bo, Y., Chen, D., Zhang, K. & Szeto, C. C. Environmental pollution to kidney disease: an updated review of current knowledge and future directions. Kidney Int. 106, 214–225 (2024).
Google Scholar
Landoni, G. et al. A randomized trial of intravenous amino acids for kidney protection. N. Engl. J. Med. 391, 687–698 (2024).
Google Scholar
Tavares, C. A. M. et al. Dapagliflozin for critically Ill patients with acute organ dysfunction: the DEFENDER randomized clinical trial. JAMA 332, 401–411 (2024).
Google Scholar
Katsuumi, G. et al. SGLT2 inhibition eliminates senescent cells and alleviates pathological aging. Nat. Aging 4, 926–938 (2024).
Google Scholar
Yanase, F. et al. Mega-dose sodium ascorbate: a pilot, single-dose, physiological effect, double-blind, randomized, controlled trial. Crit. Care 27, 371 (2023).
Google Scholar
Poyan Mehr, A. et al. De novo NAD(+) biosynthetic impairment in acute kidney injury in humans. Nat. Med. 24, 1351–1359 (2018).
Google Scholar
Zarbock, A. et al. Recommendations for clinical trial design in acute kidney injury from the 31st Acute Disease Quality Initiative consensus conference. A consensus statement. Intensive Care Med. 50, 1426–1437 (2024).
Google Scholar
Zarbock, A. et al. Designing acute kidney injury clinical trials. Nat. Rev. Nephrol. 20, 137–146 (2024).
Google Scholar
Inda-Filho, A. J., Ribeiro, H. S., Vieira, E. A. & Ferreira, A. P. Epidemiological profile of acute kidney injury in critically ill patients admitted to intensive care units: a prospective Brazilian cohort. J. Bras. Nefrol. 43, 580–585 (2021).
Google Scholar
Ponce, D., Zorzenon Cde, P., Santos, N. Y., Teixeira, U. A. & Balbi, A. L. Acute kidney injury in intensive care unit patients: a prospective study on incidence, risk factors and. Rev. Bras. Ter. Intensiv. 23, 321–326 (2011).
Google Scholar
Ephraim, R. K. D. et al. Assessment of the RIFLE criteria for the diagnosis of acute kidney injury; a retrospective study in South-western Ghana. BMC Nephrol. 17, 99 (2016).
Google Scholar
Halle, M. P. E. et al. Incidence, characteristics and prognosis of acute kidney injury in Cameroon: a prospective study at the Douala general hospital. Ren. Fail. 40, 30–37 (2018).
Google Scholar
Matyanga, P. K. G., Muchemwa, L. K. & Mujuru, H. A. Prevalence of acute kidney injury in neonates admitted at a referral hospital, Harare, Zimbabwe. Cent. Afr. J. Med. 59, 1–6 (2013).
Google Scholar
Arshad, A. & Ayaz, A. Prevalence of risk factors of acute kidney injury in a tertiary care hospital in Pakistan. J. Pak. Med. Assoc. 70, 1439–1441 (2020).
Google Scholar
Hussain, S. W. et al. Determining the incidence of acute kidney injury using the RIFLE criteria in the medical intensive care unit in a tertiary care hospital setting in Pakistan. Cureus 11, e4071 (2019).
Google Scholar
Sengthavisouk, N. et al. Epidemiology and short-term outcomes of acute kidney injury among patients in the intensive care unit in Laos: a nationwide multicenter, prospective, and observational study. BMC Med. 18, 180 (2020).
Google Scholar
Srisawat, N. et al. The epidemiology and characteristics of acute kidney injury in the Southeast Asia intensive care unit: a prospective multicentre study. Nephrol. Dial. Transpl. 35, 1729–1738 (2020).
Google Scholar
Flechet, M. et al. AKIpredictor, an online prognostic calculator for acute kidney injury in adult critically ill patients: development, validation and comparison to serum neutrophil gelatinase-associated lipocalin. Intensive Care Med. 43, 764–773 (2017).
Google Scholar
Keenswijk, W., Vanmassenhove, J., Raes, A., Dhont, E. & VandeWalle, J. Epidemiology and outcome of acute kidney injury in children, a single center study. Acta Clin. Belg. Int. J. Clin. Lab. Med. 72, 405–412 (2017).
Google Scholar
Kerr, M., Bedford, M., Matthews, B. & O’Donoghue, D. The economic impact of acute kidney injury in England. Nephrol. Dial. Transplant. 29, 1362–1368 (2014).
Google Scholar
Pickup, L. et al. The effect of admission and pre-admission serum creatinine as baseline to assess incidence and outcomes of acute kidney injury in acute medical admissions. Nephrol. Dial. Transpl. (2021).
Google Scholar
Stucker, F. et al. Risk factors for community-acquired acute kidney injury in patients with and without chronic kidney injury and impact of its initial management on prognosis: a prospective observational study. BMC Nephrol. 18, 380 (2017).
Google Scholar
Wallace, K. et al. Use of an electronic alert to identify patients with acute kidney injury. Clin. Med. 14, 22–26 (2014).
Google Scholar
Wonnacott, A., Meran, S., Amphlett, B., Talabani, B. & Phillips, A. Epidemiology and outcomes in community-acquired versus hospital-acquired AKI. Clin. J. Am. Soc. Nephrol. 9, 1007–1014 (2014).
Google Scholar
link