Sepsis criteria and kidney function: eliminating sex, age and economic status biases
No authors listed American College of Chest Physicians/Society of Critical Care Medicine Consensus Conference: definitions for sepsis and organ failure and guidelines for the use of innovative therapies in sepsis. Crit. Care Med. 20, 864–874 (1992).
Google Scholar
Levy, M. M. et al. 2001 SCCM/ESICM/ACCP/ATS/SIS International sepsis definitions conference. J. Intensive Care Med. 29, 530–538 (2003).
Google Scholar
Singer, M. et al. The Third International Consensus definitions for sepsis and septic shock (Sepsis-3). JAMA 315, 801–810 (2016).
Google Scholar
Schlapbach, L. J. et al. International consensus criteria for pediatric sepsis and septic shock. JAMA 331, 665–674 (2024).
Google Scholar
Sanchez-Pinto, L. N. et al. Development and validation of the Phoenix criteria for pediatric sepsis and septic shock. JAMA 331, 675–686 (2024).
Google Scholar
Cruz, A. T. et al. Implementation of goal-directed therapy for children with suspected sepsis in the emergency department. Pediatrics 127, e758–e766 (2011).
Google Scholar
Bernardo, E. O. et al. Community-acquired acute kidney injury among children seen in the pediatric emergency department. Acad. Emerg. Med. 25, 758–768 (2018).
Google Scholar
O’Neil, E. R. et al. Passive acute kidney injury alerts: less is not more. Pediatr. Res. 90, 496–498 (2021).
Google Scholar
Vincent, J. L. et al. The SOFA (sepsis-related organ failure assessment) score to describe organ dysfunction/failure. Intensive Care Med. 22, 707–710 (1996).
Google Scholar
Metlay, J. P. et al. Diagnosis and treatment of adults with community-acquired pneumonia. An official clinical practice guideline of the American Thoracic Society and Infectious Diseases Society of America. Am. J. Respir. Crit. Care Med. 200, e45–e67 (2019).
Google Scholar
Murugan, R. et al. Acute kidney injury in non-severe pneumonia is associated with an increased immune response and lower survival. Kidney Int. 77, 527–535 (2010).
Google Scholar
Kellum, J. A., Bellomo, R. & Ronco, C. Does this patient have acute kidney injury? An AKI checklist. Intensive Care Med. 42, 96–99 (2016).
Google Scholar
Kellum, J. A. et al. Classifying AKI by urine output versus serum creatinine level. J. Am. Soc. Nephrol. 26, 2231–2238 (2015).
Google Scholar
Kaddourah, A., Basu, R. K., Bagshaw, S. M. & Goldstein, S. L. Epidemiology of acute kidney injury in critically ill children and young adults. N. Engl. J. Med. 376, 11–20 (2017).
Google Scholar
Prowle, J. R. et al. Oliguria as predictive biomarker of acute kidney injury in critically ill patients. Crit. Care 15, R172 (2011).
Google Scholar
Leedahl, D. D. et al. Derivation of urine output thresholds that identify a very high risk of AKI in patients with septic shock. Clin. J. Am. Soc. Nephrol. 9, 1168–1174 (2014).
Google Scholar
Kaddourah, A., Basu, R. K., Goldstein, S. L., Sutherland, S. M. Oliguria and acute kidney injury in critically ill children: implications for diagnosis and outcomes. Pediatr. Crit. Care Med. 20, 332–339 (2019).
Google Scholar
Jin, K. et al. Intensive monitoring of urine output is associated with increased detection of acute kidney injury and improved outcomes. Chest 152, 972–979 (2017).
Google Scholar
Kumar, A. et al. Duration of hypotension before initiation of effective antimicrobial therapy is the critical determinant of survival in human septic shock. Crit. Care Med. 34, 1589–1596 (2006).
Google Scholar
Shankar-Hari, M. & Rubenfeld, G. D. Understanding long-term outcomes following sepsis: implications and challenges. Curr. Infect. Dis. Rep. 18, 37 (2016).
Google Scholar
Uchino, S. et al. Acute renal failure in critically ill patients: a multinational, multicenter study. JAMA 294, 813–818 (2005).
Google Scholar
Neveu, H., Kleinknecht, D., Brivet, F., Loirat, P. & Landais, P. Prognostic factors in acute renal failure due to sepsis. Results of a prospective multicentre study. Nephrol. Dial. Transpl. 11, 293–299 (1996).
Google Scholar
Silvester, W., Bellomo, R. & Cole, L. Epidemiology, management, and outcome of severe acute renal failure of critical illness in Australia. Crit. Care Med. 29, 1910–1915 (2001).
Google Scholar
Bagshaw, S. M. et al. Prognosis for long-term survival and renal recovery in critically ill patients with severe acute renal failure: a population-based study. Crit. Care 9, R700–R709 (2005).
Google Scholar
Akcan Arikan, A. et al. Resuscitation bundle in pediatric shock decreases acute kidney injury and improves outcomes. J. Pediatr. 167, 1301–1305 e1301 (2015).
Google Scholar
Fitzgerald, J. C. et al. Risk factors and inpatient outcomes associated with acute kidney injury at pediatric severe sepsis presentation. Pediatr. Nephrol. 33, 1781–1790 (2018).
Google Scholar
Fitzgerald, J. C. et al. Association of early hypotension in pediatric sepsis with development of new or persistent acute kidney injury. Pediatr. Nephrol. 36, 451–461 (2021).
Google Scholar
Kellum, J. A. et al. The effects of alternative resuscitation strategies on acute kidney injury in patients with septic shock. Am. J. Respir. Crit. Care Med. 193, 281–287 (2016).
Google Scholar
Fitzgerald, J. C. et al. Acute kidney injury in pediatric severe sepsis: an independent risk factor for death and new disability. Crit. Care Med. 44, 2241–2250 (2016).
Google Scholar
Robinson, C. et al. Serum creatinine monitoring after acute kidney injury in the PICU. Pediatr. Crit. Care Med. 22, 412–425 (2021).
Google Scholar
Schulman, I. H. et al. Readmission and mortality after hospitalization with acute kidney injury. Am. J. Kidney Dis. 82, 63–74 e61 (2023).
Google Scholar
Starr, M. C. et al. Severe acute kidney injury is associated with increased risk of death and new morbidity after pediatric septic shock. Pediatr. Crit. Care Med. 21, e686–e695 (2020).
Google Scholar
McNicholas, B., Akcan Arikan, A. & Ostermann, M. Quality of life after acute kidney injury. Curr. Opin. Crit. Care 29, 566–579 (2023).
Google Scholar
Leelahavanichkul, A. et al. Chronic kidney disease worsens sepsis and sepsis-induced acute kidney injury by releasing high mobility group box protein-1. Kidney Int. 80, 1198–1211 (2011).
Google Scholar
Doi, K. et al. Pre-existing renal disease promotes sepsis-induced acute kidney injury and worsens outcome. Kidney Int. 74, 1017–1025 (2008).
Google Scholar
Ngu, K., Reid, D. & Tobin, A. Trends and outcomes of chronic kidney disease in intensive care: a 5-year study. Intern. Med. J. 47, 62–67 (2017).
Google Scholar
Robinson, C. H. et al. Long-term kidney outcomes after pediatric acute kidney injury. J. Am. Soc. Nephrol. 35, 1520–1532 (2024).
Google Scholar
Hsu, C. Y. et al. The risk of acute renal failure in patients with chronic kidney disease. Kidney Int. 74, 101–107 (2008).
Google Scholar
Hsu, R. K., McCulloch, C. E., Dudley, R. A., Lo, L. J. & Hsu, C. Y. Temporal changes in incidence of dialysis-requiring AKI. J. Am. Soc. Nephrol. 24, 37–42 (2013).
Google Scholar
Chanchlani, R. et al. Secular trends in incidence, modality and mortality with dialysis receiving AKI in children in Ontario: a population-based cohort study. Clin. J. Am. Soc. Nephrol. 14, 1288–1296 (2019).
Google Scholar
Murugan, R., Bellomo, R., Palevsky, P. M. & Kellum, J. A. Ultrafiltration in critically ill patients treated with kidney replacement therapy. Nat. Rev. Nephrol. 17, 262–276 (2021).
Google Scholar
Formeck, C. L., Feldman, R., Althouse, A. D. & Kellum, J. A. Risk and timing of de novo sepsis in critically ill children after acute kidney injury. Kidney360 4, 308–315 (2023).
Google Scholar
Mehta, R. L. et al. Sepsis as a cause and consequence of acute kidney injury: program to improve care in acute renal disease. Intensive Care Med. 37, 241–248 (2011).
Google Scholar
Robinson, C. et al. Acute kidney injury in the pediatric intensive care unit: outpatient follow-up. Pediatr. Res. 91, 209–217 (2022).
Google Scholar
Chawla, L. S., Eggers, P. W., Star, R. A. & Kimmel, P. L. Acute kidney injury and chronic kidney disease as interconnected syndromes. N. Engl. J. Med. 371, 58–66 (2014).
Google Scholar
Kellum, J. A. et al. Use of biomarkers to identify acute kidney injury to help detect sepsis in patients with infection. Crit. Care Med. 49, e360–e368 (2021).
Google Scholar
Peerapornratana, S., Manrique-Caballero, C. L., Gomez, H. & Kellum, J. A. Acute kidney injury from sepsis: current concepts, epidemiology, pathophysiology, prevention and treatment. Kidney Int. 96, 1083–1099 (2019).
Google Scholar
Manrique-Caballero, C. L., Del Rio-Pertuz, G. & Gomez, H. Sepsis-associated acute kidney injury. Crit. Care Clin. 37, 279–301 (2021).
Google Scholar
Kuwabara, S., Goggins, E. & Okusa, M. D. The pathophysiology of sepsis-associated AKI. Clin. J. Am. Soc. Nephrol. 17, 1050–1069 (2022).
Google Scholar
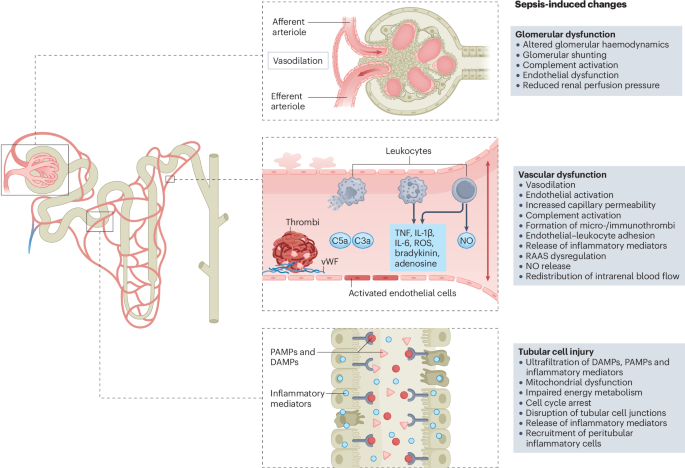
Gomez, H. et al. A unified theory of sepsis-induced acute kidney injury: inflammation, microcirculatory dysfunction, bioenergetics, and the tubular cell adaptation to injury. Shock 41, 3–11 (2014).
Google Scholar
Tanaka, S., Portilla, D. & Okusa, M. D. Role of perivascular cells in kidney homeostasis, inflammation, repair and fibrosis. Nat. Rev. Nephrol. 19, 721–732 (2023).
Google Scholar
Bhargava, P. & Schnellmann, R. G. Mitochondrial energetics in the kidney. Nat. Rev. Nephrol. 13, 629–646 (2017).
Google Scholar
Jin, K. et al. Activation of AMP-activated protein kinase during sepsis/inflammation improves survival by preserving cellular metabolic fitness. FASEB J. 34, 7036–7057 (2020).
Google Scholar
Starr, M. C. et al. Advances in pediatric acute kidney injury pathobiology: a report from the 26th Acute disease quality initiative (ADQI) conference. Pediatr. Nephrol. 39, 941–953 (2024).
Google Scholar
Bode, C., Weis, S., Sauer, A., Wendel-Garcia, P. & David, S. Targeting the host response in sepsis: current approaches and future evidence. Crit. Care 27, 478 (2023).
Google Scholar
Zarbock, A. et al. Sepsis-associated acute kidney injury: consensus report of the 28th Acute disease quality initiative workgroup. Nat. Rev. Nephrol. 19, 401–417 (2023).
Google Scholar
Legrand, M. & Kellum, J. A. Serum creatinine in the critically ill patient with sepsis. JAMA 320, 2369–2370 (2018).
Google Scholar
Kashani, K., Rosner, M. H. & Ostermann, M. Creatinine: from physiology to clinical application. Eur. J. Intern. Med. 72, 9–14 (2020).
Google Scholar
Gansevoort, R. T. et al. What should European nephrology do with the new CKD-EPI equation? Nephrol. Dial. Transpl. 38, 1–6 (2023).
Google Scholar
Nankivell, B. J., Nankivell, L. F. J., Elder, G. J. & Gruenewald, S. M. How unmeasured muscle mass affects estimated GFR and diagnostic inaccuracy. EClinicalMedicine 29-30, 100662 (2020).
Google Scholar
Rachel, M., Galiniak, S., Biesiadecki, M. & Gala-Bladzinska, A. Renal function in patients with cystic fibrosis: a single-center study. Int. J. Env. Res. Public. Health 19, 5454 (2022).
Google Scholar
Liu, K. D. et al. Acute kidney injury in patients with acute lung injury: impact of fluid accumulation on classification of acute kidney injury and associated outcomes. Crit. Care Med. 39, 2665–2671 (2011).
Google Scholar
Dixon, C. G., Thadani, S., Fitzgerald, J. C., Akcan-Arikan, A. & Yehya, N. Fluid overload precedes and masks cryptic kidney injury in pediatric acute respiratory distress syndrome. Crit. Care Med. 51, 765–774 (2023).
Google Scholar
Basu, R. K. et al. Acute kidney injury based on corrected serum creatinine is associated with increased morbidity in children following the arterial switch operation. Pediatr. Crit. Care Med. 14, e218–e224 (2013).
Google Scholar
Prowle, J. R. et al. Serum creatinine changes associated with critical illness and detection of persistent renal dysfunction after AKI. Clin. J. Am. Soc. Nephrol. 9, 1015–1023 (2014).
Google Scholar
Doi, K. et al. Reduced production of creatinine limits its use as marker of kidney injury in sepsis. J. Am. Soc. Nephrol. 20, 1217–1221 (2009).
Google Scholar
Hefny, F., Stuart, A., Kung, J. Y. & Mahmoud, S. H. Prevalence and risk factors of augmented renal clearance: a systematic review and meta-analysis. Pharmaceutics 14, 445 (2022).
Google Scholar
Bilbao-Meseguer, I., Rodriguez-Gascon, A., Barrasa, H., Isla, A. & Solinis, M. A. Augmented renal clearance in critically ill patients: a systematic review. Clin. Pharmacokinet. 57, 1107–1121 (2018).
Google Scholar
Thadani, S., Goldstein, S. & Conroy, A. L. Phoenix criteria for pediatric sepsis and septic shock. JAMA 331, 2049–2050 (2024).
Google Scholar
Boulware, L. E. & Mohottige, D. The seen and the unseen: race and social inequities affecting kidney care. Clin. J. Am. Soc. Nephrol. 16, 815–817 (2021).
Google Scholar
Smeets, N. J. L. et al. Maturation of GFR in term-born neonates: an individual participant data meta-analysis. J. Am. Soc. Nephrol. 33, 1277–1292 (2022).
Google Scholar
Schwartz, G. J. & Furth, S. L. Glomerular filtration rate measurement and estimation in chronic kidney disease. Pediatr. Nephrol. 22, 1839–1848 (2007).
Google Scholar
Kane-Gill, S. L. et al. Risk factors for acute kidney injury in older adults with critical illness: a retrospective cohort study. Am. J. Kidney Dis. 65, 860–869 (2015).
Google Scholar
Ibarz, M., Haas, L. E. M., Ceccato, A. & Artigas, A. The critically ill older patient with sepsis: a narrative review. Ann. Intensive Care 14, 6 (2024).
Google Scholar
Perazzo, S., Revenis, M., Massaro, A., Short, B. L. & Ray, P. E. A new approach to recognize neonatal impaired kidney function. Kidney Int. Rep. 5, 2301–2312 (2020).
Google Scholar
Starr, M. C. et al. Kidney health monitoring in neonatal intensive care unit graduates: a modified delphi consensus statement. JAMA Netw. Open. 7, e2435043 (2024).
Google Scholar
Shields, C. A., Wang, X. & Cornelius, D. C. Sex differences in cardiovascular response to sepsis. Am. J. Physiol. Cell Physiol. 324, C458–C466 (2023).
Google Scholar
Zhang, M. et al. Sex-based analysis of treatment responses in animal models of sepsis: a preclinical systematic review protocol. Syst. Rev. 12, 50 (2023).
Google Scholar
Curtis, L. M. Sex and gender differences in AKI. Kidney360 5, 160–167 (2024).
Google Scholar
Benavidez, G. A., Zahnd, W. E., Hung, P. & Eberth, J. M. Chronic disease prevalence in the US: sociodemographic and geographic variations by zip code tabulation area. Prev. Chronic Dis. 21, E14 (2024).
Google Scholar
Asfar, P. et al. High versus low blood-pressure target in patients with septic shock. N. Engl. J. Med. 370, 1583–1593 (2014).
Google Scholar
Phillips, D. et al. The influence of socioeconomic status on presentation and outcome of acute kidney injury. QJM 111, 849–857 (2018).
Google Scholar
Holmes, J. et al. Acute kidney injury, age, and socioeconomic deprivation: evaluation of a national data set. Kidney Int. Rep. 4, 824–832 (2019).
Google Scholar
Lameire, N. H. et al. Harmonizing acute and chronic kidney disease definition and classification: report of a kidney disease: improving global outcomes (KDIGO) consensus conference. Kidney Int. 100, 516–526 (2021).
Google Scholar
Adamson, C. et al. Initial decline (Dip) in estimated glomerular filtration rate after initiation of dapagliflozin in patients with heart failure and reduced ejection fraction: insights from DAPA-HF. Circulation 146, 438–449 (2022).
Google Scholar
Ahmad, T. et al. Worsening renal function in patients with acute heart failure undergoing aggressive diuresis is not associated with tubular injury. Circulation 137, 2016–2028 (2018).
Google Scholar
Kidney Disease: Improving Global Outcomes (KDIGO) Acute Kidney Injury Work Group. KDIGO Clinical practice guideline for acute kidney injury. Kidney Int Suppl. 2, 1–138 (2012).
Zappitelli, M. et al. Ascertainment and epidemiology of acute kidney injury varies with definition interpretation. Clin. J. Am. Soc. Nephrol. 3, 948–954 (2008).
Google Scholar
Al-Jaghbeer, M., Dealmeida, D., Bilderback, A., Ambrosino, R. & Kellum, J. A. Clinical decision support for in-hospital AKI. J. Am. Soc. Nephrol. 29, 654–660 (2018).
Google Scholar
Bataineh, A. et al. Sustained effects of a clinical decision support system for acute kidney injury. Nephrol. Dial. Transpl. 35, 1819–1821 (2020).
Google Scholar
O’Neil, E. R. et al. Defining pediatric community-acquired acute kidney injury: an observational study. Pediatr. Res. 87, 564–568 (2020).
Google Scholar
Harrison, A. M. et al. Developing the surveillance algorithm for detection of failure to recognize and treat severe sepsis. Mayo Clin. Proc. 90, 166–175 (2015).
Google Scholar
Selby, N. M. & Francis, S. T. Assessment of acute kidney injury using MRI. J. Magn. Reson. Imaging (2024).
Google Scholar
Alge, J. L. & Arthur, J. M. Biomarkers of AKI: a review of mechanistic relevance and potential therapeutic implications. Clin. J. Am. Soc. Nephrol. 10, 147–155 (2015).
Google Scholar
Meena, J., Thomas, C. C., Kumar, J., Mathew, G. & Bagga, A. Biomarkers for prediction of acute kidney injury in pediatric patients: a systematic review and meta-analysis of diagnostic test accuracy studies. Pediatr. Nephrol. 38, 3241–3251 (2023).
Google Scholar
Goldstein, S. L. et al. Derivation and validation of an optimal neutrophil gelatinase-associated lipocalin cutoff to predict stage 2/3 acute kidney injury (AKI) in critically ill children. Kidney Int. Rep. 9, 2443–2452 (2024).
Google Scholar
Kashani, K. et al. Discovery and validation of cell cycle arrest biomarkers in human acute kidney injury. Crit. Care 17, R25 (2013).
Google Scholar
Hoste, E. et al. Identification and validation of biomarkers of persistent acute kidney injury: the RUBY study. Intensive Care Med. 46, 943–953 (2020).
Google Scholar
Fiorentino, M. et al. Serial measurement of cell-cycle arrest biomarkers [TIMP-2]·[IGFBP7] and risk for progression to death, dialysis, or severe acute kidney injury in patients with septic shock. Am. J. Respir. Crit. Care Med. 202, 1262–1270 (2020).
Google Scholar
Kellum, J. A. & Goldstein, S. L. Do novel biomarkers have utility in the diagnosis and prognosis of AKI? PRO. Kidney360 4, 1663–1666 (2023).
Google Scholar
Meersch, M. et al. Prevention of cardiac surgery-associated AKI by implementing the KDIGO guidelines in high risk patients identified by biomarkers: the PrevAKI randomized controlled trial. Intensive Care Med. 43, 1551–1561 (2017).
Google Scholar
Goldstein, S. L. et al. Real-time acute kidney injury risk stratification-biomarker directed fluid management improves outcomes in critically ill children and young adults. Kidney Int. Rep. 8, 2690–2700 (2023).
Google Scholar
Dorshow, R. B., Debreczeny, M. P., Goldstein, S. L. & Shieh, J. J. Clinical validation of the novel fluorescent glomerular filtration rate tracer agent relmapirazin (MB-102). Kidney Int. 106, 679–687 (2024).
Google Scholar
Dorshow, R. B. et al. Transdermal detection of MB-102 and correlation to meropenem pharmacokinetics during continuous renal replacement therapy: in vivo results. ASAIO J. 69, 708–715 (2023).
Google Scholar
Dorshow, R. B., Debreczeny, M. P. & Goldstein, S. L. GFR measurement utilizing transdermal detection methodology. J. Am. Soc. Nephrol. (2025).
Google Scholar
Cameron, J. S. A history of urine microscopy. Clin. Chem. Lab. Med. 53 (Suppl. 2), s1453–s1464 (2015).
Google Scholar
Bagshaw, S. M. et al. A prospective evaluation of urine microscopy in septic and non-septic acute kidney injury. Nephrol. Dial. Transpl. 27, 582–588 (2012).
Google Scholar
Becker, G. J., Garigali, G. & Fogazzi, G. B. Advances in urine microscopy. Am. J. Kidney Dis. 67, 954–964 (2016).
Google Scholar
Basu, R. K. et al. Combining functional and tubular damage biomarkers improves diagnostic precision for acute kidney injury after cardiac surgery. J. Am. Coll. Cardiol. 64, 2753–2762 (2014).
Google Scholar
Norris, N. et al. Liberal fluid resuscitation is associated with improved outcomes in pediatric acute pancreatitis. J. Pediatr. 276, 114329 (2024).
Google Scholar
Inker, L. A. et al. New creatinine- and cystatin C-based equations to estimate GFR without race. N. Engl. J. Med. 385, 1737–1749 (2021).
Google Scholar
Kotani, Y., Fujii, T., Uchino, S., Doi, K. & Group, J. S. Modification of sequential organ failure assessment score using acute kidney injury classification. J. Crit. Care 51, 198–203 (2019).
Google Scholar
link