Epidemiological trend in diabetic kidney disease (DKD) burden in China from 1990 to 2021, and projections for 2041: an analysis of the global burden of disease study 2021 | BMC Public Health

Descriptive analysis (The burden of DKD in the China between 1990 and 2021)
In China, there were 6321(95% CI: 3949,9464) new cases in 2021 and 20,688(95% CI: 15277,27014) deaths due to DKD caused by type 1 diabetes (DKD-T1DM). Age-standardized rates in terms of prevalence (ASPR), incidence (ASIR), mortality (ASMR), DALYs, YLDs, and YLLs of DKD-T1DM in 2021 were 28.32 cases (95% CI: 23.95,33.23) per 100,000, 0.7 new cases (95% CI: 0.38,1.14) per 100,000, 1.06 deaths (95% CI: 0.79,1.38) per 100,000, 47.95 DALYs (95% CI: 36.9,60.73) per 100,000, 4.55 YLDs (95% CI: 3,6.25) per 100,000, and 43.4 YLLs (95% CI:33.05,55.97) per 100,000. The all-age numbers and age-standardized rates for males and females are presented in Table 1. It is clear that men have a higher incidence, deaths, DALYs, and YLLs than women (Table 1).
In China, there were 354,157 (95% CI: 321265,382784) new cases in 2021 and 107,652 (95% CI: 84626,134047) deaths due to DKD caused by type 2 diabetes (DKD-T2DM). Age-standardized rates in terms of prevalence (ASPR), incidence (ASIR), mortality (ASMR), DALYs, YLDs, and YLLs of DKD-T2DM in 2021 were 1053.92 cases (95% CI: 971.11,1139.64) per 100,000, 16.29 new cases (95% CI: 14.92,17.53) per 100,000, 5.64 deaths (95% CI: 4.46,7) per 100,000, 122.15 DALYs (95% CI: 99.62,146.99) per 100,000, 23.3 YLDs (95% CI: 16.29,30.54) per 100,000, and 98.85 YLLs (95% CI:78.16,123.45) per 100,000 (Table 2). The all-age numbers and age-standardized rates for males and females are presented in Table 2. There was no significant difference in the disease burden of DKD-T2DM between men and women.
Figure 1 shows the prevalence, incidence, mortality numbers of DKD-T1DM(A, C, E) and DKD-T2DM(B, D, F) for the different age groups in China in 2021. Figure 2 shows the age-standardized prevalence, incidence, and mortality rates of DKD for the different age groups in China in 2021. DKD-T1DM is more prevalent in people aged 45–59, and it increases quickly between the ages of 20 and 54.In patients with DKD-T1DM, the incidence showed a completely different trend, the younger the age, the higher the incidence. The 50–59 age group has the highest mortality rate for DKD-T1DM. DKD-T2DM is more prevalent in people aged 45–79, and it increases quickly between the ages of 60 and 79. In terms of DKD-T2DM incidence, similar tendencies are observed; there is a high incidence in people aged 65–74, with a substantial increase in incidence occurring between the ages of 60 and 74. Another notable phenomenon is the sharp rise in the incidence rate of DKD-T2DM among Male patients in the 85–94 age group. The 70–79 age group has the highest mortality rate for DKD-T2DM. Among female patients, the mortality rate shows a persistent upward trend with advancing age. Age-standardized DALYs, YLDs, and YLLs rates showed similar trends by sex and age group (Supplementary Fig. 1, 2).
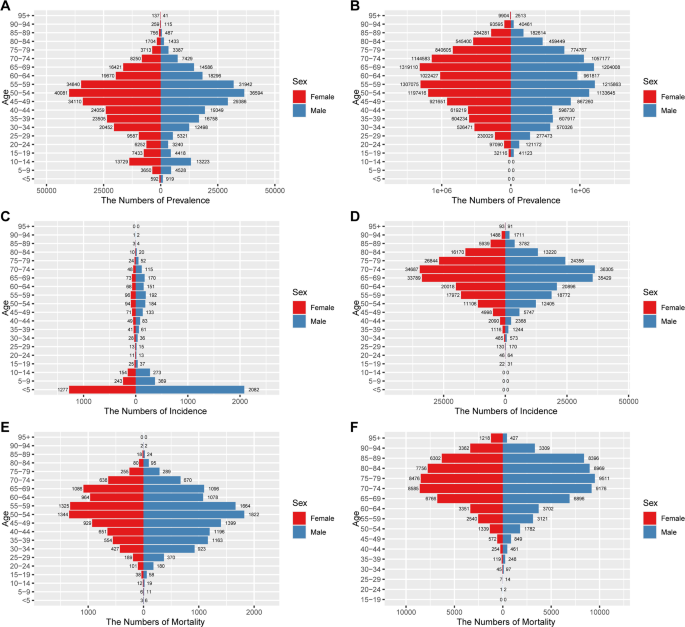
Age-specific numbers prevalence, incidence, and mortality rates of DKD in China, 2021. A Age-specific prevalence number of DKD-T1DM. B Age-specific prevalence number of DKD-T2DM. C Age-specific incidence number of DKD-T1DM.(D) Age-specific incidence number of DKD-T2DM. E Age-specific mortality number of DKD-T1DM. F Age-specific mortality number of DKD-T2DM
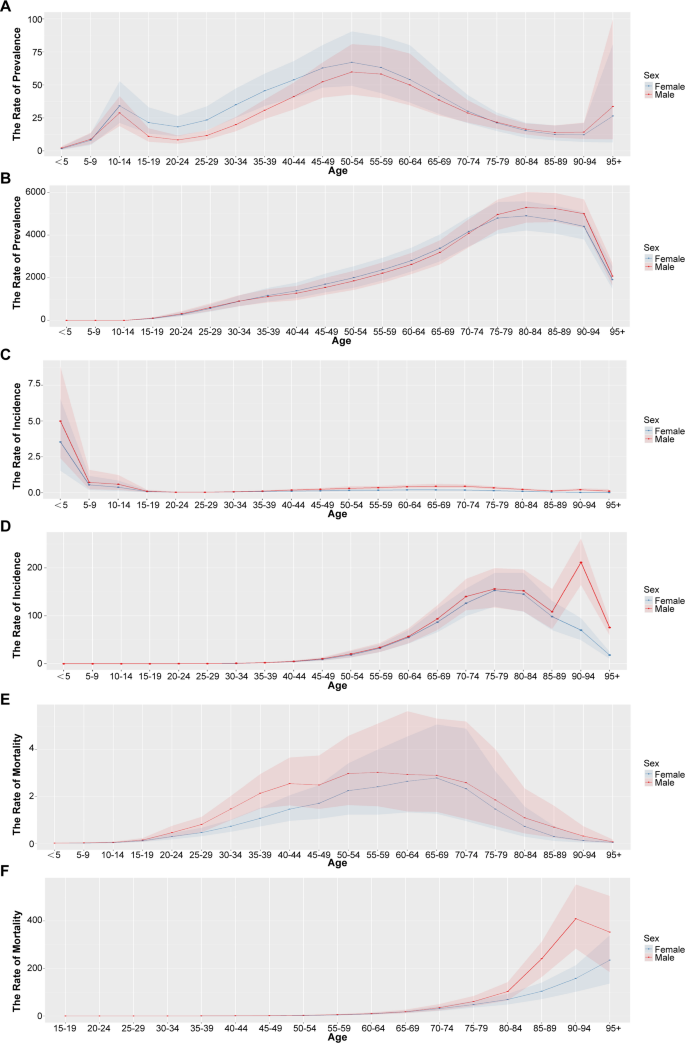
Age-standardized prevalence, incidence, and mortality rates of DKD in China, 2021. A Age-standardized prevalence rate of DKD-T1DM. B Age-standardized prevalence rate of DKD-T2DM. C Age-standardized incidence rate of DKD-T1DM. D Age-standardized incidence rate of DKD-T2DM. E Age-standardized mortality rate of DKD-T1DM. F Age-standardized mortality rate of DKD-T2DM
Between 1990 and 2021, age-standardized mortality rates (ASMR) for DKD-T1DM and DKD-T2DM in China declined: DKD-T1DM ASMR decreased from 1.8 (95% CI: 1.42, 2.25) to 1.06 (95% CI: 0.79, 1.38) per 100,000, while DKD-T2DM ASMR fell from 6.83 (95% CI: 5.74, 8.34) to 5.64 (95% CI: 4.46, 7) per 100,000. The age-standardized DALY of DKD-T1DM in China decreased from 80.92 (95% CI: (65.12,98.39) per 100,000 people in 1990 to 47.95 (95% CI: 36.9,60.73) per 100,000 people in 2021. The age-standardized DALY of DKD-T2DM in China decreased from 155.94(95% CI: (131.16,188.26) per 100,000 people in 1990 to 122.15 (95% CI: 99.62,146.99) per 100,000 people in 2021 (Supplementary Tables 1 and Supplementary Table 2). When compared to global data, China’s DKD burden has changed significantly.
Figure 3 depicts the trends in the sex-specific all-age number and age-standardized rates of DKD prevalence, incidence and mortality in China between 1990 and 2021. The sex-specific, age-standardized incidence and mortality rates for DKD fluctuated by calendar year. The DKD-T1DM prevalence is generally increasing (Fig. 3A), while mortality is gradually declining (Fig. 3E). In DKD-T1DM both the male and female age-standardized DALYs are decreasing. However, it seems there is no decrease in the number of DALYs for men (Fig. 3G).In DKD-T2DM, the number of prevalence and incidence are generally increasing, while the rate of prevalence and incidence show a steady trend (Fig. 3B, D). The number of mortalities and DALYs are generally increasing, while the rate of mortality and DALYs show a descending trend (Fig. 3F, H). Supplementary Figs. 3 present the sex-specific all-age number and age-standardized rates of YLDs and LLDs in China.
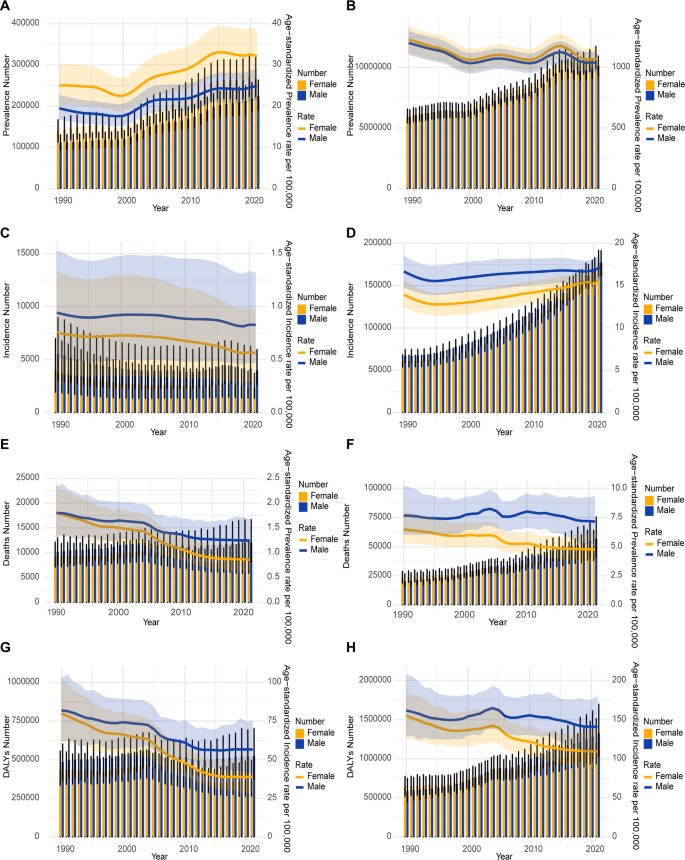
Trends in the all-age cases and age-standardized incidence, mortality, and DALYs rates of DKD by sex from 1990 to 2021. A Prevalence number and rate of DKD-T1DM.(B)Prevalence number and rate of DKD-T2DM. C Incidence number and rate of DKD-T1DM. D Incidence number and rate of DKD-T2DM. E Mortality number and rate of DKD-T1DM. F Mortality number and rate of DKD-T2DM. G DALYs number and rate of DKD-T1DM. H DALYs number and rate of DKD-T2DM
Joinpoint regression analysis
Joinpoint regression analyses of the age-standardized prevalence, incidence, mortality rates for DKD in China between 1990 and 2021 are shown in Figs. 4, 5 and 6. We found the DKD-T1DM prevalence trend significantly increased from 2000 until 2005 in both female (APC = 4.19 (2000–2005), 95% CI: 3.89,4.47) (Fig. 4C) and male (APC = + 4.34 (2000–2005), 95% CI: 4.10,4.52) (Fig. 4E) populations. Since 2014, the prevalence trend has moderated in both sexes, the decline being particularly pronounced in females. DKD-T1DM incidence trended differently from prevalence, showing a consistent annual decline. The sharpest reduction occurred between 2015 and 2018 (females: APC=−3.49, 95% CI: −3.73 to −3.07; males: APC=−2.20, 95% CI: −2.49 to −1.72) (Fig. 5C and E). The trend in the mortality rate of DKD-T1DM also showed a downward trend, with the most pronounced reduction observed between 2004 and 2007 in both female (APC = −5.64 (2004–2007), 95% CI: −7.02,−4.25) (Fig. 6C) and male (APC = −4.40 (2004–2007), 95% CI: −5.46,−3.33) (Fig. 6E) populations. Supplementary Table 3 shows the AAPCs in DKD-T1DM prevalence, incidence, and mortality rates over three decades. Age-standardized prevalence, incidence and mortality rates for DKD-T1DM in China changed by 0.79 (95% CI: 0.75,0.85), −0.62 (95% CI: −0.66,−0.59), and − 1.72(95% CI: ,−1.53), respectively, between 1990 and 2021. Surprisingly, males had a lower AAPC of incidence, prevalence, and mortality rates than females.
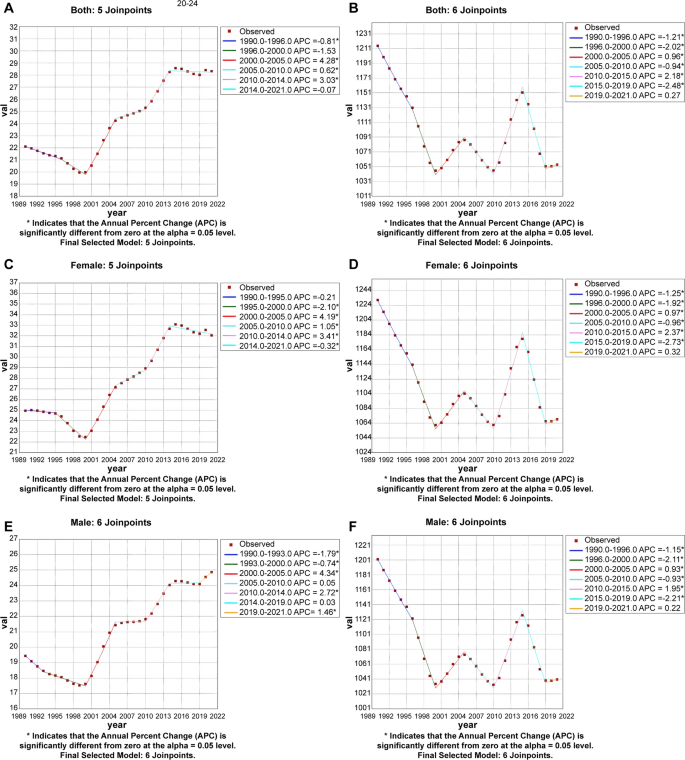
Joinpoint regression analysis of the sex-specific age-standardized prevalence rate for DKD in China from 1990 to 2021. A Age-standardized prevalence rate for both sex of DKD-T1DM. B Age-standardized prevalence rate for both sex of DKD-T2DM. C Age-standardized prevalence rate for female of DKD-T1DM. D Age-standardized prevalence rate for female of DKD-T2DM. E Age-standardized prevalence rate for males of DKD-T1DM. F Age-standardized prevalence rate for males of DKD-T2DM
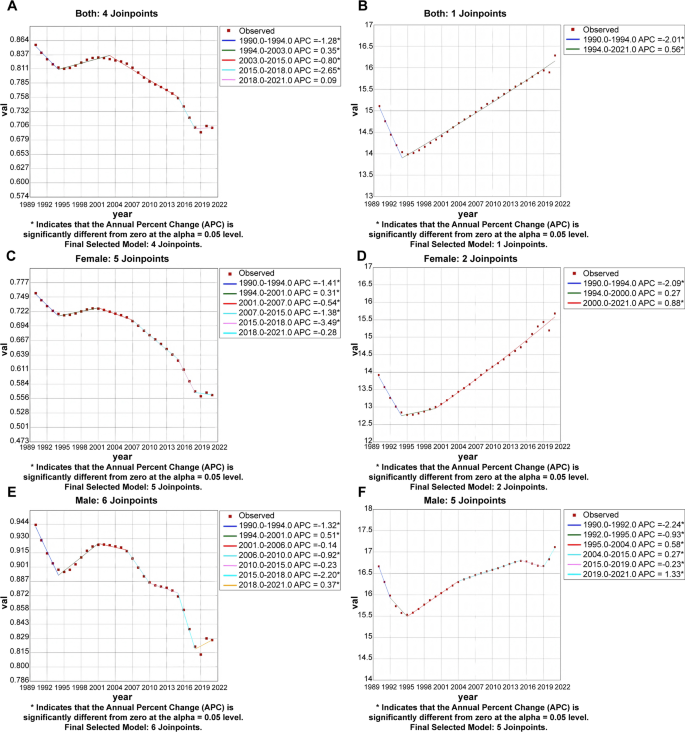
Joinpoint regression analysis of the sex-specific age-standardized incidence rate for DKD in China from 1990 to 2021. A Age-standardized incidence rate for both sex of DKD-T1DM. B Age-standardized incidence rate for both sex of DKD-T2DM. C Age-standardized incidence rate for female of DKD-T1DM. D Age-standardized incidence rate for female of DKD-T2DM (E)Age-standardized incidence rate for males of DKD-T1DM. F Age-standardized incidence rate for males of DKD-T2DM
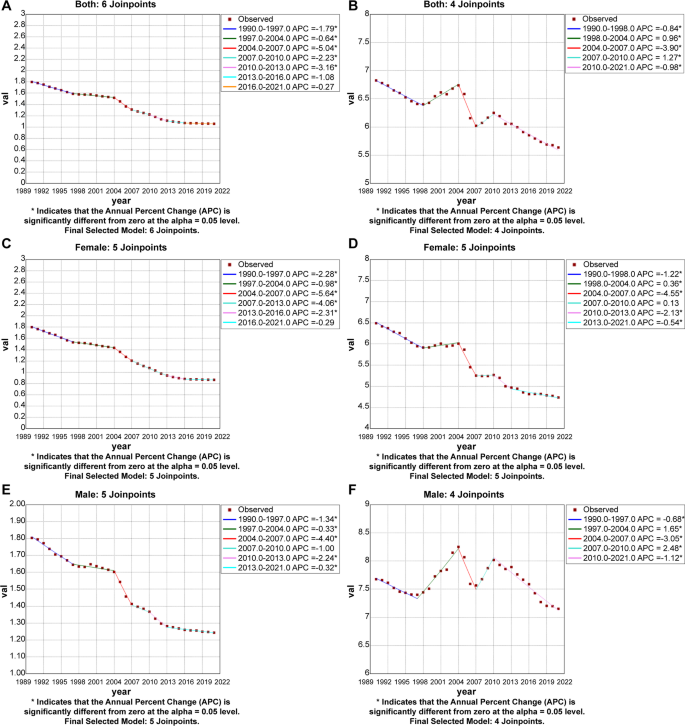
Joinpoint regression analysis of the sex-specific age-standardized mortality rate for DKD in China from 1990 to 2021. A Age-standardized mortality rate for both sex of DKD-T1DM. B Age-standardized mortality rate for both sex of DKD-T2DM. C Age-standardized mortality rate for female of DKD-T1DM. D Age-standardized mortality rate for female of DKD-T2DM. E Age-standardized mortality rate for males of DKD-T1DM. F Age-standardized mortality rate for males of DKD-T2DM
We found the DKD-T2DM prevalence trend descended between 1990 and 2000 in both female (APC=−1.92(1996–2000), 95% CI: −2.24,−1.66) (Fig. 4D) and male (APC=−2.11(1996–2000), 95% CI: −2.40,−1.88) (Fig. 4F) populations. However, the prevalence showed fluctuating changes between 2000 and 2021, with the most obvious upward trend from 2010 to 2015 in both sexes (APC = 2.18 (2010–2015), 95% CI: 2.02,2.34). The incidence showed first a decline and then a rise, with the inflection point in 1994 and 1995, with the greatest increase observed between 2000 and 2021 in females (APC = 0.88(2000–2021), 95% CI: 0.84,0.96) (Fig. 5D), and the greatest increase observed between 2019 and 2021 in males (APC = 1.33(2019–2021), 95% CI: 1.16,1.48) (Fig. 5F). The trend in the mortality rate of DKD-T2DM also showed a downward trend in females, with the most pronounced reduction observed between 2004 and 2007 (APC=−4.55(2004–2007), 95% CI: −5.92,−3.15) (Fig. 6D). The Male mortality rate showed a fluctuating trend, with the most increase in 2007–2010 (APC = 2.48(2007–2010),95% CI:0.65,4.33) and the most significant decrease in 2004–2007 (APC=−3.05(2004–2007),95% CI:−4.77,−1.30) (Fig. 6F). Supplementary Table 4 shows the AAPCs in DKD-T2DM prevalence, incidence, and mortality rates over three decades. Age-standardized prevalence, incidence and mortality rates for DKD-T2DM in China changed by −0.46(95% CI:−0.49,−0.42), 0.22(95% CI:0.20,0.26), and − 0.64 (95% CI: −0.82,−0.47).
Age, period and cohort effects on DKD mortality and incidence
Figures 7 and 8 illustrate the age-period-cohort effect of DKD mortality and incidence rate. In China, with regard to the age effect within the same birth cohort, the mortality rate of DKD-T1DM peaks in the 40–55 age group, while the mortality rate of DKD-T2DM increases with age (Fig. 7AB). The incidence of DKD-T1DM was highest at 2.5 years old(Rate:3.84,95%CI: 3.27,4.42), and showed a sharp decline in the age range of the 2.5–7.5 age group, followed by a relatively flat fluctuation, while the DKD-T2DM showed an upward trend followed by a downward trend, reaching a peak in the age group of the 72–83 age group (Fig. 8AB). With regard to the period effect, the mortality rates in both the DKD-T1DM and DKD-T2DM populations steadily decreased (Fig. 7CD). The incidence of the DKD-T1DM population showed an increasing trend, while the incidence of the DKD-T2DM population was relatively stable (Fig. 8CD). Regarding the cohort effect, the mortality rate of DKD did not change significantly, showing a small downward trend (Fig. 7EF). The incidence of DKD-T1DM showed a gradual increasing trend, with the highest incidence in the 1997–2002 cohort(RR = 1.70 (1997), 95% CI: 1.45,2.00)t(RR = 1.73 (2002), 95% CI: 1.47,2.04). Overall incidence of DKD-T2DM showed an initial increase and then decreased, with a relatively high incidence in the 1962–1977 cohort(RR = 1.03 (1962), 95% CI: 1.01,1.05)(RR = 1.05 (1967), 95% CI: 1.03,1.08)(RR = 1.04 (1972), 95% CI: 1.01,1.08)(RR = 1.03 (1977), 95% CI: 0.98,1.08) (Fig. 8EF). Supplementary Tables 5–10 provide the specific data for the age-period-cohort analysis of the incidence, mortality, and prevalence rates of DKD in China.Supplementary Fig. 4 exhibits the age-period-cohort effect of DKD prevalence. The net drifts in mortality for both the DKD-T1DM and DKD-T2DM populations were less than 0 (−1.99% and-1.50%, respectively, p < 0.001) (Fig. 7GH).
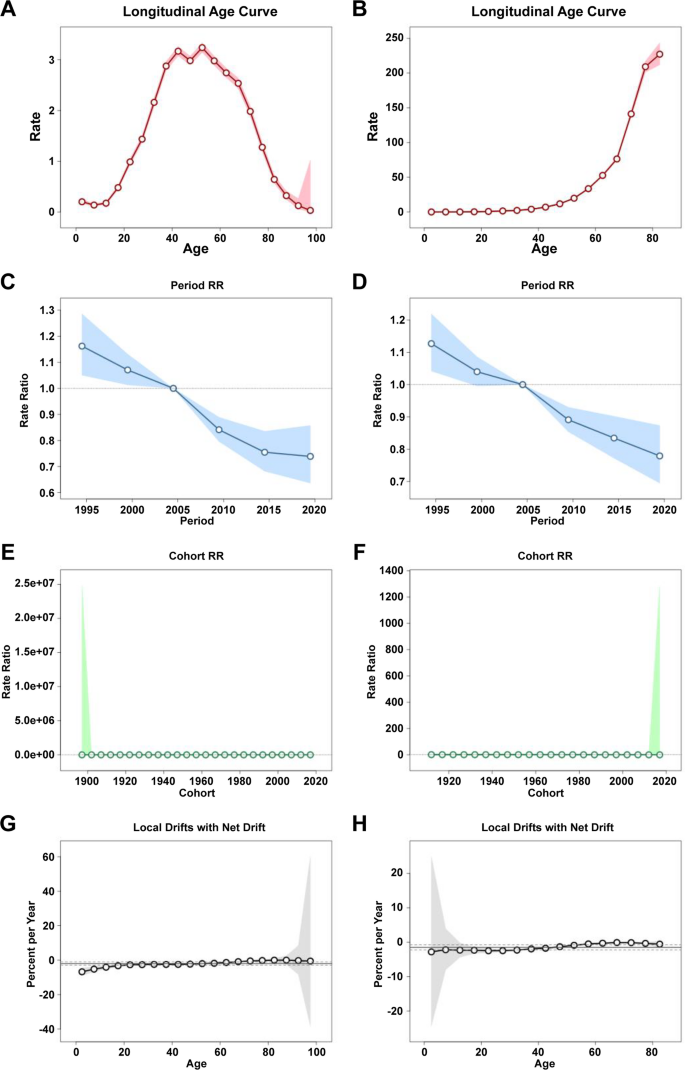
The trends in the mortality associated with long age, period RR, cohort RR, local drift of DKD from 1990 to 2021. A Long age of DKD-T1DM. B Long age of DKD-T2DM. C Period RR of DKD-T1DM. D Period RR of DKD-T2DM. E Cohort RR of DKD-T1DM. F Cohort RR of DKD-T2DM. G Local drift of DKD-T1DM. H Local drift of DKD-T2DM
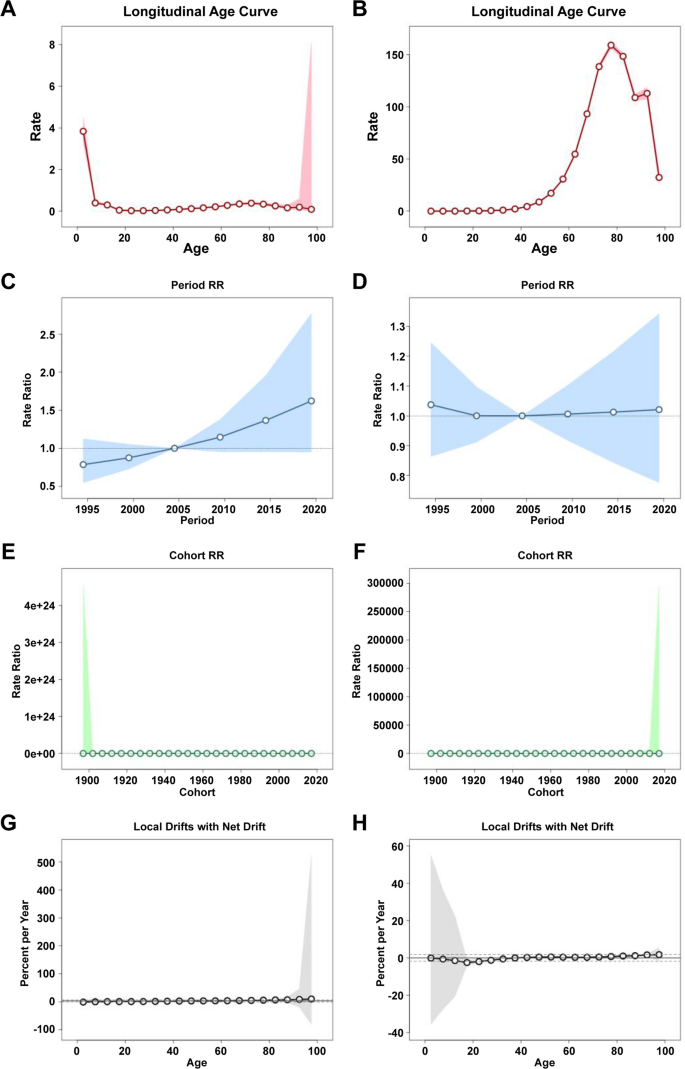
The trends in the incidence associated with long age, period RR, cohort RR, local drift of DKD from 1990 to 2021. A Long age of DKD-T1DM. B Long age of DKD-T2DM. C Period RR of DKD-T1DM. D Period RR of DKD-T2DM.(E)Cohort RR of DKD-T1DM. F Cohort RR of DKD-T2DM. G Local drift of DKD-T1DM. H Local drift of DKD-T2DM
Decomposition analysis of DKD burden
Decomposition analysis was employed to quantify the relative contributions of age structure changes, population size changes, and epidemiological changes to the incidence and mortality number of DKD (Fig. 9; Tables 3 and 4). The past 30 years have seen a decrease in incidence of Chinese DKD-T1DM, with consistent trends in both men and women. In DKD-T1DM, aging and epidemiological change accounted for 89.5% and 57.57% of the decrease in incidence, respectively; the effect of population growth on incidence decrease was negative (−47.07%). The incidence of DKD-T2DM in the Chinese population has seen a significant increase. In DKD-T2DM, aging, population growth and epidemiological change accounted for 75.04%, 19.22% and 5.74% of the increase in incidence, respectively. Over the past 30 years, the mortality rate of female patients with DKD-T1DM has decreased, while the mortality rate of male patients has increased. In female DKD-T1DM, aging and population growth accounted for 588.17% and 266.45% of the decrease in mortality, respectively; the effect of epidemiological change on mortality decrease was negative (−954.62%). In male DKD-T1DM, aging and population growth accounted for 210.38% and 105.99% of the increase in mortality, respectively; the effect of epidemiological change on mortality increase was negative (−216.37%). Mortality in Chinese patients with DKD-T2DM has seen a significant increase. In DKD-T2DM, aging and population growth accounted for 93.86% and 23.92% of the decrease in mortality, respectively; the effect of epidemiological change in mortality increase was negative (−17.79%).
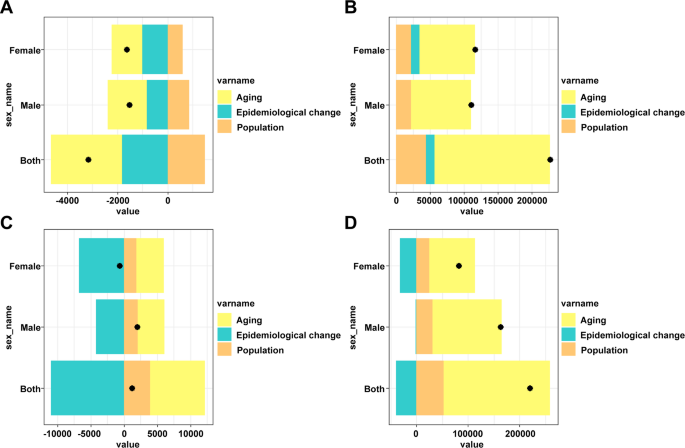
The relative contributions of aging, population, and epidemiological changes to the number of incidence, mortality and DALYs from 1990 to 2021,comparison in different genders. A Incidence of DKD-T1DM. B Incidence of DKD-T2DM. C Mortality of DKD-T1DM. D Mortality of DKD-T2DM. Note: The black dot represents the overall difference of incidence, mortality and DALYs from 1990 to 2021
Prediction of DKD epidemiological trends in the next twenty years
The ARIMA model was used to quantitatively depict the trends of DKD age-standardized mortality, prevalence and incidence over the next 20 years (Fig. 10, Supplementary Fig. 5,6). The optimized model was chosen to be (0,1,2) for DKD-T1DM mortality, with an AIC value of −177.16 after being filtered by the auto.arima()function. Q–Q plots, ACF and PACF plots revealed that the residual error was normally distributed (Supplementary Fig. 7). The Ljung-Box test confirmed that the residuals of the model were white noise (χ2 = 0.55, P = 0.97). By repeating the aforementioned steps, the ARIMA model (0,1,1) for DKD-T2DM age-standardized mortality (AIC=−61.02) was developed. It also was proven robust by the Ljung-Box test (χ2 = 4.72, P = 0.45). ASMR in DKD-T1DM is expected to decrease from 1.06(95% CI: 0.79–1.38) per 100,000 in 2021 to 0.60(95% CI: 0.32–0.88) per 100,000 in 2041. ASMR still showed a downward trend in DKD-T2DM; it is expected to decrease from 5.64(95% CI: 4.46-7.00) per 100,000 in 2021 to 4.84(95% CI: 3.66–6.02) per 100,000 in 2041 (Supplementary Tables 11–18).
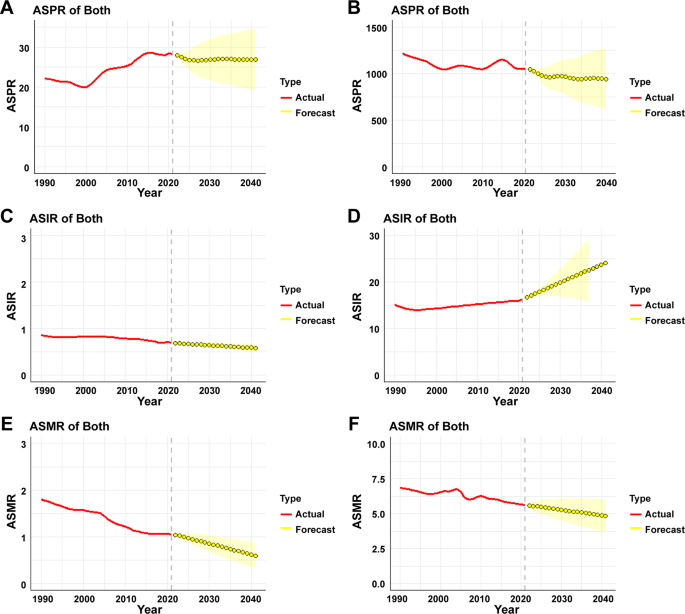
Predicted trends of DKD prevalence, incidence and mortality in China over 20 years (2022–2041) (A)Trends of DKD prevalence of DKD-T1DM. (B)Trends of DKD prevalence of DKD-T2DM (C)Trends of DKD incidence of DKD-T1DM. (D)Trends of DKD incidence of DKD-T2DM (E)Trends of DKD mortality of DKD-T1DM. (F)Trends of DKD mortality of DKD-T2DM
The optimized model was chosen to be (2,1,0) for DKD-T1DM age-standardized prevalence, with an AIC value of −5.54 after being filtered by the auto.arima()function. Q-Q plots, ACF and PACF plots revealed that the residual error was normally distributed (Supplementary Fig. 8). The Ljung-Box test confirmed that the residuals of the model were white noise (χ2 = 1.68, P = 0.79). By repeating the aforementioned steps, the ARIMA model (3,1,0) for DKD-T2DM age-standardized prevalence rate (AIC=−183.32) was developed; it also was proven robust by the Ljung-Box test (χ2 = 2.13, P = 0.55). It is predicted that ASPR in DKD-T1DM will not fluctuate much in the next 20 years; ASPR was 28.32(95% CI: 23.95–33.22) per 100,000 in 2021 and is predicted to be 26.90(95% CI: 19.16–34.63) per 100,000 in 2041. However, the trend of ASPR in DKD-T2DM is predicted to decrease slightly; it is expected to decrease from 10.54(95% CI: 9.71–11.40)‰ in 2021 to 9.41(95% CI: 6.14–12.69)‰ in 2041 (Supplementary Tables 11–18).
The optimized model was chosen to be (0,1,1) for DKD-T1DM age-standardized incidence, with an AIC value of 233.23 after being filtered by the auto.arima()function. Q-Q plots, ACF and PACF plots revealed that the residual error was normally distributed (Supplementary Fig. 9). The Ljung-Box test confirmed that the residuals of the model were white noise (χ2 = 1.67, P = 0.89) (Supplementary Table 12). By repeating the aforementioned steps, the ARIMA model (0,2,0) for DKD-T2DM age-standardized incidence rate (AIC=−57.96) was developed; it also was proven robust by the Ljung-Box test (χ2 = 0.42, P = 0.99). The trend of ASIR in DKD-T1DM is predicted to decrease slightly; it is expected to decrease from 0.70(95% CI: 0.38–1.14) per 100,000 in 2021 to 0.58(95% CI: 0.50–0.67) per 100,000 in 2041. However, it is predicted that ASIR in DKD-T2DM will show an obvious upward trend; it will increase from 16.29(95% CI: 14.92–17.53) per 100,000 in 2021 to 24.14(95% CI: 14.78–33.50) per 100,000 in 2041 (Supplementary Tables 14 and Supplementary Table 18).Projections are based on the continuation of trends observed between 1990 and 2021. Widespread adoption of renoprotective agents or enhanced diabetes screening in the future may result in a lower incidence of DKD-T2DM than predicted.
The ARIMA models of prevalence, incidence and mortality of T1DM-DKD and T2DM-DKD in different genders are shown in Supplementary Figs. 5 and 6, and their Q-Q plots and ACF and PACF plots are also shown(Supplementary Fig. 7–12). The actual data and forecast data of ASPR, ASIR and ASMR for Males and females are also shown in Supplementary Tables 1414 and Supplementary Table 18. The predictive capacity of ARIMA models is Listed in Supplementary Tables 1313 and Supplementary Table 17.
link