Comparative study on the effects of high fat diet and capsicum diet on the digestive organs of guinea pigs
Dietary behaviours of individuals substantially influence overall health outcomes. Maintaining a balanced and nutritious diet is essential for promoting physiological well-being. The prevalence of unhealthy eating habits has created considerable challenges for public health, resulting in various conditions, including gastrointestinal and cardiovascular diseases. Numerous studies have emphasised the risk associated with high-fat diets, which endanger the health of digestive organs and other organ systems. Chronic consumption of such diets has been associated with health complications, including indigestion, fatty liver disease, atherosclerosis, and cerebrovascular incidents, including strokes. Despite the established risks associated with high-fat dietary patterns, the literature on the health effects of chilli consumption has predominantly focused on its potential role in disease prevention and therapeutic uses. capsicums and their bioactive constituents are frequently cited for their potential benefits, including weight control, analgesic effects, and antibacterial properties. An increasing discourse indicates that chilli may exert beneficial and detrimental effects on human health. This investigation was initiated by an inquiry into the disparate effects of different dietary habits on the health of digestive system organs.
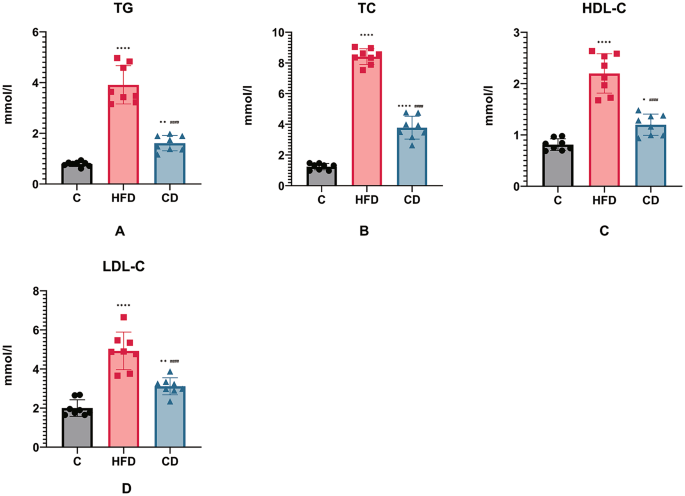
Our research indicates that prolonged consumption of high-fat and chilli-based diets can significantly disrupt blood lipid metabolism. This disruption is marked by abnormal increases in TG, total cholesterol (TC), high-density lipoprotein cholesterol (HDL-C), and low-density lipoprotein cholesterol (LDL-C). A previous study demonstrated that long-term high-fat diets are significant causes of blood lipid metabolism disorders9.TG, TC, HDL-C, and LDL-C are essential markers of lipid metabolism. Triglycerides are essential for energy storage and safeguarding of internal organs; however, elevated TG levels may signify the onset of metabolic diseases, including hyperlipidaemia, diabetes, and cardiovascular conditions10. TC represents the overall level of cholesterol present in all lipoproteins in the bloodstream. Abnormal increases in TC levels are closely associated with hyperlipidaemia, atherosclerosis, coronary heart disease, stroke, and other cardiovascular diseases11. HDL-C is primarily synthesised in the liver and is essential in transporting phospholipids and cholesterol. HDL-C exerts anti-atherosclerotic and cardiovascular benefits through various mechanisms, including facilitating cholesterol reverse transport, antioxidation, and anti-inflammation. Numerous studies have demonstrated a negative correlation between HDL-C levels and the incidence of coronary heart disease. However, a previous study demonstrated that conditions including chronic hepatitis and fatty liver can cause elevated HDL-C levels12. Conversely, hyperlipoproteinemia, acute myocardial infarction, coronary heart disease, and diabetes are closely associated with abnormal increases in LDL-C levels. Studies have demonstrated a significant positive correlation between LDL-C concentrations and the risk of coronary heart disease. Herein, the high-fat diet group exhibited abnormal increases in serum TG, TC, HDL-C, and LDL-C, confirming that long-term high-fat diets can impair lipid metabolism. Additionally, numerous studies demonstrated that capsicum diets or capsaicin intake may help improve lipid metabolic disorders13,14. However, there is a lack of studies on the impact of a high capsicum intake on blood lipids. Our study demonstrates that a long-term chilli-based diet can lead to abnormal increases in serum TG, TC, HDL-C, and LDL-C. This effect is probably associated with pathological liver damage and inflammatory changes in the intestines induced by the chilli diet, which disrupt cholesterol metabolism15,16,17,18,19. Furthermore, numerous studies have demonstrated that cholesterol is secreted from the liver into the intestines via bile, a process closely associated with bile acids and intestinal microbiota20,21,22,23. However, the specific mechanism by which prolonged chilli intake disrupts serum cholesterol metabolism, and whether this is mediated by bile acid metabolism or gut microbiota, requires further comprehensive investigation.
Our investigation demonstrated that the long-term high-fat and chilli-based diet intake can elicit inflammatory responses in the serum, characterised by significant elevations in pro-inflammatory cytokines, specifically TNF-α, IL-1β, and IL-6. These cytokines are essential in the inflammatory process, and substantial evidence from existing literature indicates that prolonged high-fat diet intake fosters inflammatory responses within the serum. Tan’s research highlights that an increased intake of dietary fats leads to excessive accumulation of free fatty acids in the bloodstream, which subsequently incites oxidative stress, thereby promoting systemic inflammation24. Furthermore, Binayi et al. reported that high-fat diets induce endoplasmic reticulum stress, which impairs lipid metabolism and subsequently triggers inflammatory pathways25. Malesza et al. reported that extended high-fat diet intake can lead to dysbiosis of gut microbiota and impairments in intestinal barrier function, facilitating the translocation of metabolic byproducts from harmful bacteria into the circulatory system, exacerbating systemic inflammation26. Our findings are consistent with those of previous studies, reinforcing that long-term high-fat diet intake is associated with increased inflammatory responses. Conversely, although it is a common belief that diets enriched with capsicum provide health benefits, primarily through the activation of the transient receptor potential vanilloid 1 (TRPV1) receptor signalling pathway, which is believed to attenuate inflammation and alleviate pain, literature documenting the potential inflammatory effects of prolonged capsicum intake is scarce27. Xiang et al. reported that high doses of capsaicin may induce intestinal inflammation, potentially attributable to alterations in gut microbiota composition28. Our research extends these findings by demonstrating that a prolonged diet high in capsicum diets induces inflammatory responses in the serum and adversely affects the digestive organs, substantiating the adverse consequences of sustained capsicum intake on gastrointestinal health.
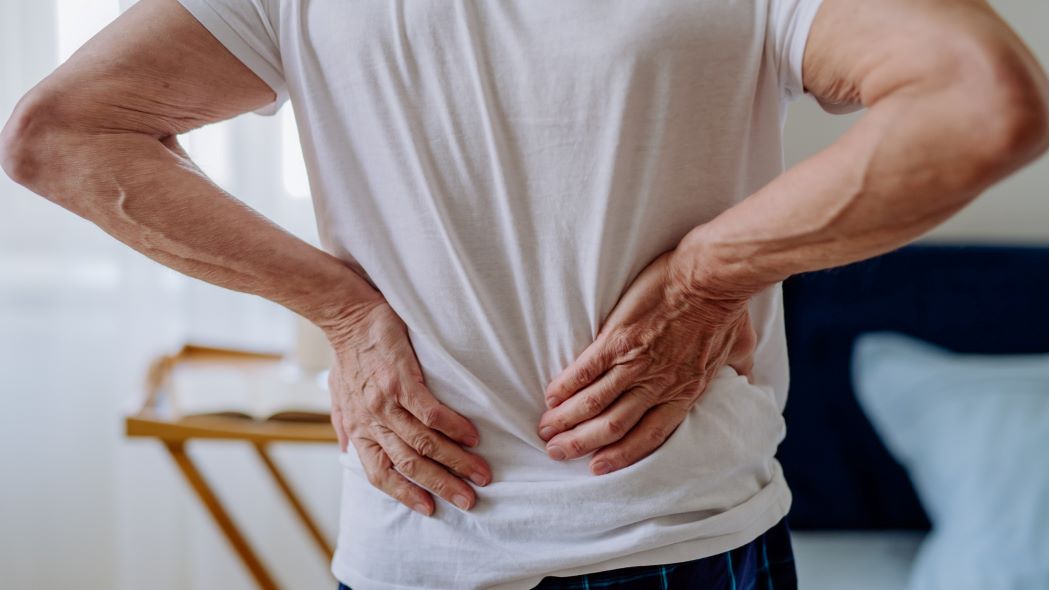
Studies demonstrated that prolonged consumption of high-fat foods and capsicum diets can significantly damage gastric tissue. This damage is primarily characterised by injury to the gastric mucosa, inflammatory responses, and the ensuing development of ulcers. In comparing the effects of high-fat diets to those resulting from long-term exposure to capsicum diets, the gastric mucosa exposed to long-term capsicum diets exhibit more severe manifestations, including increased ulceration, atrophy, and necrosis. The stomach is essential to the digestive system; it is responsible for food storage and mechanical and chemical digestion processes, which are facilitated by gastric motility, acid secretion, and pepsin activity. Numerous academic studies have suggested a direct correlation between high-fat diets and the onset of gastritis, although the precise mechanisms underlying this association are inadequately clarified. Some researchers suggest that this association may arise from lipotoxicity, which compromises the stability of gastric mucosal organelles and gastric tissue integrity, thereby inducing gastritis and precancerous transformations in gastric tissue29. Additionally, obesity, frequently associated with high-fat consumption, has been associated with pathological alterations in gastric tissue. An increase in the quantity of ghrelin-expressing cells in the stomach is posited to correlate closely with obesity mechanisms induced by high-fat diets30,31,32. Our research has confirmed the deleterious effects of high-fat diets on gastric tissue; however, the extent to which this impact is due to lipid toxicity, as opposed to other contributing factors, requires further investigation. The current literature indicates a duality in the effects of capsicum diets. Many scholars assert that capsicum diets and their derivatives exhibit anticancer and antioxidant properties and therapeutic potential for gastric cancer treatment. This functionality may be significantly associated with the activation of the TRPV1 receptor signalling pathway33,34. However, some researchers have empirically demonstrated a correlation between elevated capsicum diets and specific gastric conditions, including gastric bleeding35. Increasing evidence indicates that a higher intake of capsicum diets or capsaicin can markedly elevate the risk of developing gastric cancer36,37,38. Our research has concluded that long-term capsicum consumption adversely affects gastric tissue. The underlying mechanisms contributing to this impact are closely associated with inflammatory processes and immune responses; however, the specific pathways involved require further investigation.
Studies demonstrate that prolonged high-fat food intake causes substantial damage to liver tissue. This damage is predominantly characterised by liver steatosis, fibrosis, and the onset of inflammatory processes. However, prolonged intake of capsaicin leads to liver steatosis and mild fibrosis, although without significant inflammatory alterations compared to prolonged high-fat diet intake. The liver is the primary metabolic and digestive organ. It is essential in glucose and lipid metabolism and bile production and secretion. Extensive studies have demonstrated the deleterious effects of high-fat diets on liver health, confirming that long-term adherence to such dietary patterns results in fat accumulation, fibrosis, and progression of conditions including fatty liver39,40,41, chronic hepatitis42, and cirrhosis43,44. Our findings confirm the consensus that prolonged high-fat dietary intake precipitates fatty liver and hepatitis, thereby enhancing the understanding of its detrimental effects on liver function. Conversely, there is a widespread belief regarding the health benefits of capsicum diet consumption. Research indicates that capsaicin, a bioactive compound found in capsicum diets, may possess therapeutic potential in alleviating cholestatic liver fibrosis and preventing hepatotoxic injury45,46. A previous study has demonstrated that capsaicin can inhibit hepatic fat accumulation in murine models of non-alcoholic fatty liver disease induced by a high-fat diet47. Xie et al. reported that capsaicin suppresses the stemness of liver progenitor cells and inhibits liver cancer development through the SIRT1/SOX2 signalling pathway48. These findings indicate that dietary capsaicin may confer protective effects against liver fibrosis, diminish hepatic fat accumulation, and impede the onset of liver malignancies. However, the investigation into the potential adverse effects of chronic dietary capsaicin on liver health is limited. Our research indicates that long-term intake of capsicum diets may negatively impact liver function, indicating that dietary capsaicin possesses a dualistic nature regarding human health, with potential long-term adverse effects outweighing its benefits, possibly associated with inflammatory responses.
Our investigation revealed the detrimental effects of a high-fat and chilli-based diet on the gallbladder mucosa, specifically resulting in its atrophy. The gallbladder is essential for the storage, concentration, and secretion of bile, a substance vital to cholesterol metabolism. Research indicates that a moderate intake of dietary fats can stimulate normal gallbladder contraction, facilitating the timely release of bile and decreasing bile stagnation, thereby reducing the risk of gallstone formation and exacerbation of cholecystitis. Numerous studies confirm that prolonged high-fat intake may impair gallbladder contractility49,50although the underlying mechanisms are unclear. Furthermore, extensive research has demonstrated that high-fat diets significantly increase the prevalence of cholesterol gallstone formation51,52. Our findings indicate that prolonged high-fat dietary patterns correlate with atrophy of the gallbladder mucosa, frequently serving as the primary pathological basis for conditions including chronic cholecystitis and gallstone disease. Many studies have demonstrated that prolonged consumption of chilli-based diets can adversely affect gallbladder health. Studies have specifically identified excessive intake of red capsicums as a risk factor for long-term gallstone formation and gallbladder cancer, especially among Chilean women53,54. Our investigation indicates that prolonged consumption of capsicums correlates with damage to the gallbladder mucosa, suggesting a significant role of persistent capsicum intake in the pathogenesis of chronic cholecystitis and other gallbladder-related disorders.
This study demonstrated significant implications of long-term dietary patterns involving high-fat and capsicum diets on colon health. Specifically, we observed that a prolonged high-fat diet can result in colon tissue atrophy and stimulate inflammatory responses, and significant accumulation of adipocytes beneath the mucosal layer of the colon. The colon is essential to the digestive system, serving in essential nutrient absorption, including vitamins, water, and minerals, and in faeces formation. Furthermore, the symbiotic bacteria and microorganisms residing within the colon are essential in maintaining metabolic homeostasis in the digestive system. Existing literature has demonstrated that high-fat diets induce oxidative stress within the colonic mucosa, leading to enhanced permeability of the epithelial barrier and the subsequent onset of colonic mucosal inflammation55. Our findings confirm the detrimental effects of prolonged high-fat diets on colon tissue, which seem to be associated with oxidative stress-related inflammatory processes within the colonic environment. However, further investigation into the specific underlying mechanisms is required. A dichotomy of perspectives exists regarding the effect of long-term capsicum consumption on colon health. Some scholars posit that dietary capsicums may adversely affect the colon. Engel et al. (2012) demonstrated that capsaicin, the active compound in capsicums, activates the TRPV1 receptor, resulting in an increased release of calcitonin gene-related peptide and substance P, potentially contributing to the pathogenesis of colitis56. However, other researchers support the possible protective effects of capsicums and capsaicin against colonic diseases, including colitis. Kihara et al. reported that capsaicin could ameliorate dextran sulphate sodium-induced colitis through TRPV1 receptor activation57. Additionally, Mi et al. reported a significant correlation between the frequency of chilli consumption and the incidence of colitis58. This study supports the previous perspective, indicating that prolonged capsicum intake may jeopardise colon health. The underlying mechanisms for these observations may be attributed to factors including oxidative stress and inflammation; however, a more comprehensive analysis is essential to clarify the precise processes involved.
The limitations of this study are primarily focused on its analysis of the effects of high-fat and chilli diets on the morphological alterations in digestive organ tissues. The research notably failed to investigate the underlying mechanisms that may correlate inflammation, lipid metabolism, and the resultant damage to digestive organs. Future investigations should consider integrating lipidomics, proteomics, molecular biology, and other multi-omics methodologies. These comprehensive methodologies would facilitate a multi-dimensional analysis, yielding deeper insights into the key pathological mechanisms involved.
This study demonstrated that prolonged high-fat and chilli-based diet intake may adversely affect digestive organs, including the liver, stomach, gallbladder, and colon. The underlying mechanism seems to be closely associated with inflammatory responses, which cause damage to these organs and subsequently impair cholesterol metabolism. This impairment may further exacerbate lipid metabolic disorders. Although inflammation is a crucial factor in various pathological processes, the specific mechanisms require additional investigation. This research highlights the detrimental effects of prolonged chilli consumption on digestive health to inform dietary recommendations for optimal human health.
link