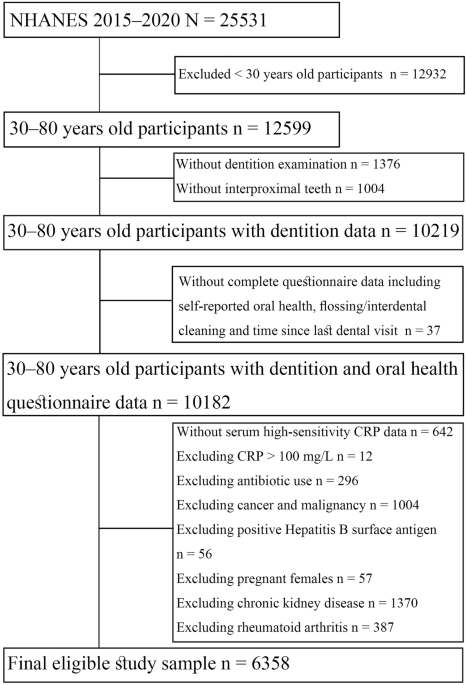
Association of participant reported oral health, tooth loss, interdental cleaning and dental visits with serum CRP
Petersen, P. E. & Ogawa, H. The global burden of periodontal disease: towards integration with chronic disease prevention and control. Periodontol 2000 60, 15–39. (2012).
Google Scholar
Sun, R. et al. Global and regional trends in prevalence of untreated caries in permanent teeth: Age-period-cohort analysis from 1990 to 2019 and projections until 2049. J. Dent. 147, 105122. (2024).
Google Scholar
Aida, J. et al. Reasons for permanent tooth extractions in Japan. J. Epidemiol 16, 214–219. (2006).
Google Scholar
Chestnutt, I. G., Binnie, V. I. & Taylor, M. M. Reasons for tooth extraction in Scotland. J. Dent. 28, 295–297. (2000).
Google Scholar
Zhang, J., Huang, X., Lu, B., Zhang, C. & Cai, Z. Can apical periodontitis affect serum levels of CRP, IL-2, and IL-6 as well as induce pathological changes in remote organs?. Clin. Oral Investig. 20, 1617–1624. (2016).
Google Scholar
Dominy, S. S. et al. Porphyromonas gingivalis in Alzheimer’s disease brains: Evidence for disease causation and treatment with small-molecule inhibitors. Sci. Adv. 5, eaau3333. (2019).
Google Scholar
Furusho, H. et al. Dental infection of Porphyromonas gingivalis exacerbates high fat diet-induced steatohepatitis in mice. J. Gastroenterol 48, 1259–1270. (2013).
Google Scholar
Brun, A. et al. Oral microbiota and atherothrombotic carotid plaque vulnerability in periodontitis patients. A cross-sectional study. J. Periodontal Res. 56, 339–350. (2021).
Google Scholar
Berlin-Broner, Y., Febbraio, M. & Levin, L. Association between apical periodontitis and cardiovascular diseases: a systematic review of the literature. Int. Endod J. 50, 847–859. (2017).
Google Scholar
Liljestrand, J. M. et al. Association of Endodontic Lesions with Coronary Artery Disease. J. Dent Res. 95, 1358–1365. (2016).
Google Scholar
Garrido, M. et al. Elevated Systemic Inflammatory Burden and Cardiovascular Risk in Young Adults with Endodontic Apical Lesions. J. Endod 45, 111–115. (2019).
Google Scholar
Gomes, M. S. et al. Can apical periodontitis modify systemic levels of inflammatory markers? A systematic review and meta-analysis. J. Endod 39, 1205–1217. (2013).
Google Scholar
Sun, J. et al. Association between C-Reactive protein and periodontitis in an obese population from the NHANES 2009–2010. BMC Oral Health 23, 512. (2023).
Google Scholar
Meisel, P. et al. Competing interplay between systemic and periodontal inflammation: obesity overrides the impact of oral periphery. Clin. Oral Investig. 25, 2045–2053. (2021).
Google Scholar
Ioannidou, E., Swede, H. & Dongari-Bagtzoglou, A. Periodontitis predicts elevated C-reactive protein levels in chronic kidney disease. J. Dent. Res. 90, 1411–1415. (2011).
Google Scholar
Lee, J. H. & Mun, S. J. Relationship between C-reactive protein level and periodontitis and systemic diseases. J. Periodontol 95, 494–501. (2024).
Google Scholar
Slade, G. D. et al. Relationship between periodontal disease and C-reactive protein among adults in the Atherosclerosis Risk in Communities study. Arch. Intern. Med. 163, 1172–1179. (2003).
Google Scholar
Bretz, W. A. et al. Systemic inflammatory markers, periodontal diseases, and periodontal infections in an elderly population. J. Am. Geriatr. Soc. 53, 1532–1537. (2005).
Google Scholar
Paraskevas, S., Huizinga, J. D. & Loos, B. G. A systematic review and meta-analyses on C-reactive protein in relation to periodontitis. J. Clin. Periodontol 35, 277–290. (2008).
Google Scholar
Garrido, M. et al. C-reactive protein expression is up-regulated in apical lesions of endodontic origin in association with interleukin-6. J. Endod 41, 464–469. (2015).
Google Scholar
Zhang, Y., Leveille, S. G. & Edward, J. Wisdom teeth, periodontal disease, and C-reactive protein in US adults. Public Health 187, 97–102. (2020).
Google Scholar
Casagrande, S. S. & Lawrence, J. M. Cardiovascular disease risk factors and their associations with inflammation among US adolescents: NHANES, 2015 to March 2020. BMJ Open Diabetes Res. Care 12, e004148. (2024).
Google Scholar
Alim, B. A., Canturk, E. & Koksal, C. The effect of treated apical periodontitis before heart valve surgery on C-reactive protein levels. Oral Dis. 27, 632–638. (2021).
Google Scholar
Garrido, M. et al. Reduced C-reactive protein levels after root canal treatment in clinically healthy young apical periodontitis individuals at cardiovascular risk. A prospective study. Int. Endod J. 57, 406–415. (2024).
Google Scholar
Al-Abdulla, N. et al. Successful endodontic treatment reduces serum levels of cardiovascular disease risk biomarkers-high-sensitivity C-reactive protein, asymmetric dimethylarginine, and matrix metalloprotease-2. Int. Endod J. 56, 1499–1516. (2023).
Google Scholar
Bakhsh, A., Moyes, D., Proctor, G., Mannocci, F. & Niazi, S. A. The impact of apical periodontitis, non-surgical root canal retreatment and periapical surgery on serum inflammatory biomarkers. Int. Endod J. 55, 923–937. (2022).
Google Scholar
Caribe, P. M. V. et al. Influence of the treatment of periodontal disease in serum concentration of sirtuin 1 and mannose-binding lectin. J. Periodontol 91, 900–905. (2020).
Google Scholar
Haworth, S. et al. Tooth loss is a complex measure of oral disease: Determinants and methodological considerations. Community Dent. Oral Epidemiol 46, 555–562. (2018).
Google Scholar
Cheng, F. et al. Tooth loss and risk of cardiovascular disease and stroke: A dose-response meta analysis of prospective cohort studies. PLoS ONE 13, e0194563. (2018).
Google Scholar
Abnet, C. C. et al. Tooth loss is associated with increased risk of total death and death from upper gastrointestinal cancer, heart disease, and stroke in a Chinese population-based cohort. Int. J. Epidemiol 34, 467–474. (2005).
Google Scholar
Vedin, O. et al. Tooth loss is independently associated with poor outcomes in stable coronary heart disease. Eur. J. Prev. Cardiol. 23, 839–846. (2016).
Google Scholar
Lee, H. J., Choi, E. K., Park, J. B., Han, K. D. & Oh, S. Tooth Loss Predicts Myocardial Infarction, Heart Failure, Stroke, and Death. J. Dent. Res. 98, 164–170. (2019).
Google Scholar
Kotronia, E. et al. Poor Oral Health and Inflammatory, Hemostatic, and Cardiac Biomarkers in Older Age: Results From Two Studies in the UK and USA. J. Gerontol A Biol. Sci. Med. Sci. 76, 346–351. (2021).
Google Scholar
Hung, H. C. et al. The association between tooth loss and coronary heart disease in men and women. J. Public Health Dent. 64, 209–215. (2004).
Google Scholar
Tu, Y. K. et al. Associations between tooth loss and mortality patterns in the Glasgow Alumni Cohort. Heart 93, 1098–1103. (2007).
Google Scholar
Hiratsuka, T. et al. Contribution of systemic inflammation and nutritional status to the relationship between tooth loss and mortality in a community-dwelling older Japanese population: a mediation analysis of data from the Tsurugaya project. Clin. Oral Investig. 24, 2071–2077. (2020).
Google Scholar
Meurman, J. H., Janket, S. J., Qvarnstrom, M. & Nuutinen, P. Dental infections and serum inflammatory markers in patients with and without severe heart disease. Oral Surg. Oral Med. Oral Pathol. Oral Radiol. Endod. 96, 695–700. (2003).
Google Scholar
Liljestrand, J. M. et al. Missing Teeth Predict Incident Cardiovascular Events, Diabetes, and Death. J. Dent. Res. 94, 1055–1062. (2015).
Google Scholar
Schwahn, C. et al. Missing, unreplaced teeth and risk of all-cause and cardiovascular mortality. Int. J. Cardiol. 167, 1430–1437. (2013).
Google Scholar
Holmlund, A., Holm, G. & Lind, L. Number of teeth as a predictor of cardiovascular mortality in a cohort of 7,674 subjects followed for 12 years. J. Periodontol. 81, 870–876. (2010).
Google Scholar
Luo, H. et al. Oral Health, Diabetes, and Inflammation: Effects of Oral Hygiene Behaviour. Int. Dent. J. 72, 484–490. (2022).
Google Scholar
Yu, Y. H., Steffensen, B., Chasman, D. I. & Buring, J. E. Self-reported oral health is associated with systemic health outcomes and all-cause mortality. J. Am. Dent. Assoc. 155, 233–243. (2024).
Google Scholar
Marchesan, J. T. et al. Flossing Is Associated with Improved Oral Health in Older Adults. J. Dent. Res. 99, 1047–1053. (2020).
Google Scholar
Chaffee, B. W., Persai, D. & Vora, M. V. Interdental Cleaning and Oral Health Status in an Adult Cohort, 2015 to 2018. J. Dent. Res. 99, 1150–1156. (2020).
Google Scholar
Marchesan, J. T. et al. Interdental Cleaning Is Associated with Decreased Oral Disease Prevalence. J. Dent. Res. 97, 773–778. (2018).
Google Scholar
Cepeda, M. S., Weinstein, R., Blacketer, C. & Lynch, M. C. Association of flossing/inter-dental cleaning and periodontitis in adults. J. Clin. Periodontol 44, 866–871. (2017).
Google Scholar
Axelsson, P., Nystrom, B. & Lindhe, J. The long-term effect of a plaque control program on tooth mortality, caries and periodontal disease in adults. Results after 30 years of maintenance. J. Clin. Periodontol. 31, 749–757. (2004).
Google Scholar
Kim, Y. H. et al. Oral health behaviors and metabolic syndrome: the 2008–2010 Korean National Health and Nutrition Examination Survey. Clin. Oral Investig. 18, 1517–1524. (2014).
Google Scholar
Moradpour, F. et al. Prevalence of metabolic syndrome and its association with oral health: First results from the Kurdish cohort study. Health Sci. Rep. 6, e1602. (2023).
Google Scholar
Xu, K. et al. Association between dental visit behavior and mortality: a nationwide longitudinal cohort study from NHANES. Clin. Oral Investig. 28, 37. (2023).
Google Scholar
Park, S. Y. et al. Improved oral hygiene care attenuates the cardiovascular risk of oral health disease: a population-based study from Korea. Eur. Heart J. 40, 1138–1145. (2019).
Google Scholar
Han, S. J. The Use of Interdental Care Products in Korean Adults Aged 30 Years and Older and Factors Affecting Their Use: 4th to 7th Korean National Health and Nutrition Examination Survey. Int. J. Environ. Res. Public Health 19, 8639. (2022).
Google Scholar
Fleming, E. B., Nguyen, D., Afful, J., Carroll, M. D. & Woods, P. D. Prevalence of daily flossing among adults by selected risk factors for periodontal disease-United States, 2011–2014. J. Periodontol 89, 933–939. (2018).
Google Scholar
Liang, L. & Aris, I. M. Minimal changes in daily flossing behavior among US adults from 2009 through 2020. J. Am. Dent. Assoc 155, 587-596.e2. (2024).
Google Scholar
Ronis, D. L., Lang, W. P., Farghaly, M. M. & Passow, E. Tooth brushing, flossing, and preventive dental visits by Detroit-area residents in relation to demographic and socioeconomic factors. J. Public Health Dent 53, 138–145. (1993).
Google Scholar
Inker, L. A. et al. New Creatinine- and Cystatin C-Based Equations to Estimate GFR without Race. N. Engl. J. Med. 385, 1737–1749. (2021).
Google Scholar
Nanri, H. et al. Association between dietary pattern and serum C-reactive protein in Japanese men and women. J. Epidemiol 21, 122–131. (2011).
Google Scholar
Zhou, W. et al. Association of Interdental Cleaning Frequency With Tooth Loss and Self-Rated Oral Health: A Cross-Sectional Study. Int. Dent. J. 75, 100803. (2025).
Google Scholar
Arabi, A. et al. Association between Serum Vitamin D Status and Circadian Syndrome: A Cross-Sectional Study. Nutrients 16, 2111. (2024).
Google Scholar
Liu, C., Hua, L. & Xin, Z. Synergistic impact of 25-hydroxyvitamin D concentrations and physical activity on delaying aging. Redox Biol. 73, 103188. (2024).
Google Scholar
Stekhoven, D. J. & Buhlmann, P. MissForest–non-parametric missing value imputation for mixed-type data. Bioinformatics 28, 112–118. (2012).
Google Scholar
Li, Y. et al. Association of periodontitis, tooth loss, and self-rated oral health with circadian syndrome in US adults: a cross-sectional population study. BMC Oral Health 25, 713. (2025).
Google Scholar
van der Weijden, F. & Slot, D. E. Oral hygiene in the prevention of periodontal diseases: the evidence. Periodontol 2000 55, 104–123. (2011).
Google Scholar
link